Rule #5: Let your baby cry for up to 12 minutes each night before it goes to sleep.
Note: Online it says 5-10 minutes instead of 12: “I do stress that some babies will fight sleep and they should be allowed 5-10 minutes crying down period.” I don’t see much of a difference in this – it remains a form of CIO.
Well, I have far too many words already written on the cry-it-out (CIO) method which is being advocated here so let’s try for a brief, succinct summary. First, think about this for yourself: Imagine you crying every night for 12 minutes because you wanted to be held and comforted by someone due to fear, stress, overstimulation, whatever and that person abandoned you. You may stop crying, but would you stop needing that affection? I doubt it and the same goes for baby. Second, we know that the cessation of crying is not related to “self-soothing” but rather infants who stop crying after CIO continue to have high cortisol responses at nighttime (at least in the short term) indicative of continued stress
Better rule? Put your baby to sleep gently and with compassion. It may involve nursing to sleep, rocking to sleep, going to sleep with your baby, or putting your baby down half asleep and letting him/her fall asleep on her own. The key point is to follow your baby’s cues on this and if you have sleep “problems” look into the reasons behind them because it is likely you will find the real cause and be able to treat it.
Rule #6: Avoid making eye contact with your baby after 10 p.m.
Note: This is also supported by Ms. Ford’s comments on her site in which she says, “I suggest avoiding eye contact at 10pm and during night feeds to help you show your baby gently that this is not playtime.”
I can only assume this is the similar type of rule to #3 about not letting baby sleep past 7 a.m. If you don’t interact, won’t your baby just sleep? Well, first off, the same things I mentioned in rule #3 about schedules are still relevant here. However, we also have to add the issue that avoiding eye contact is just downright cruel to a baby or, well, anyone. Avoiding eye contact is also one way to eliminate teaching our babies as even very young babies use eye gaze and contact to learn about many things in the world, including what our actions mean and what they need to take from it[6]. Granted eye gaze and eye contact are only a couple of the pedagogical cues our children use, but they are important ones. Furthermore, removing eye contact is one way to stop interactions with our babies and when our babies are not given the type of reciprocal interaction they expect from a loving caregiver, they tend to get even more upset[7]. Notably, touch can reduce the distress at the lack of engagement, but it does not fully eliminate it[8]. So what benefit does it gain to avoid eye contact? Well, not much that I can think of unless the goal is to try and make your child give up on trying to communicate or engage with you and I fail to see how that’s a good thing at any time.
Better rule? Use your eye contact and eye gaze to communicate with your baby[6]. Make sure your baby knows you are there for him/her and that you will listen to what your baby is trying to tell you. Then you set the stage for life-long communication which is something you really do want, especially as your child ages.
Rule #7: Do not cuddle your baby to sleep while it is feeding.
Note: Again, this is mentioned as one of her rules online as she states, “And, crucially, there is a difference between cuddling your baby and cuddling him to sleep. If he gets used to being cuddled to sleep, it will create a dependence that you will have to break at some point – and it is much easier to get him used to settling himself to sleep at three weeks of age than three months or three years.” Oddly she ignores that actually it’s not “creating a dependence” but following an evolutionary instinct.
This is one of the more popular pieces of advice given out to parents in Western societies and makes zero sense. The idea is that you’re creating a “bad habit”. Forget that this is what babies have been doing for the history of humankind up to a couple hundred years go, it literally makes no sense. First, for those of us who breastfeed, how do you feed your baby and not cuddle? I realize it’s possible, but it can be very awkward. Even those babies on a bottle, are they in charge of holding it themselves as newborns? Regardless, all this ignores (a) the very real need for infants to feel secure and safe in order to fall asleep and one of the primary ways in which they feel safe and secure is to be cuddled (you can read more on this here) and (b) the role of tryptophan in the sleep cycle. Trytophan is naturally occurring in breastmilk and occurs in larger doses at night in order to help induce sleep for infants and also leads to serotonin synthesis and development which helps a variety of cognitive functions[9][10][11]. Most babies will need comfort to fall asleep, especially in the early months and to not provide it is to not be responsive to your child’s needs. Eventually they will all learn to fall asleep independently, but how long this takes will vary child to child, with some doing it at three months, some at three years, and some even later. So long as this is not a problem for the family, it simply isn’t a problem, and for those for whom it is a problem, early sleep training in the first six months (including this pattern of refusing comfort to sleep) has been found to not only not to reliably work, but also to raise the risk of other problems[5].
Better rule? Cuddle and comfort your child as s/he needs it. Nurse your child to sleep. If any of these things stop working for you and your family and your child is old enough, you can look into gentle sleep solutions (like here for example) to help your family while respecting your child.
Rule #8: Do not let your baby share your bed.
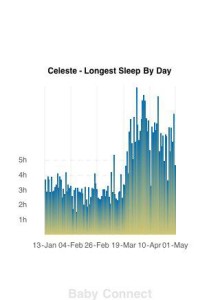
According to this rule, for most of human history we’ve done things “wrong” and many other cultures still continue to do things “wrong”, but I can’t solely blame Ms. Ford as it’s a common recommendation, but one that needs to be discussed. First, given the importance of breastfeeding to infant development, one cannot discount how bedsharing facilitates breastfeeding (for a review of the research by Dr. Helen Ball, see [12]). Second, bedsharing often facilitates greater sleep for mom and isn’t this one of the larger concerns we have in our modern day society? This image was shared with me by a mom who switched to bedsharing from room-sharing and maps the longest sleep stretch she had:
The longest sleep stretch is important because total duration of sleep does not inform on whether or not a mother received full cycles of sleep which are vital to cognitive functioning. The disruption of sleep, or rather the disruption of the sleep cycle, is linked to worsened neurobehavioural performance[13] and higher anxiety and depression[14]. Now there are safety concerns that are always brought up in the popular press; however, bedsharing can be done safely provided one does it with intention and makes sure there is a safe sleep environment for the baby (see here, here, here, and [12] for more information). Furthermore, some babies simply will not sleep without contact with a parent and telling these parents to not do what is necessary to sleep and stay functioning is asking for parents to take on a burden of exhaustion, depression, and for their babies to take on not being comforted, not sleeping themselves, and for both, hours of tears.
Better rule? Find a sleep situation that works for you and your family and make sure it is as safe as possible. What works for one family will not work for another, and that includes bedsharing (if you want to assess whether it’s for you, you can read here for some questions to ask yourself). Don’t compare your baby to other babies because they are all different and remember to be responsive to your child as it often makes your life easier too.
***
There you go. Eight rules and eight rebuttals. As I said, I sincerely hope these are misinterpreted rules but regardless they are ones that pervade our society and deserve discussion. Remember: Your baby needs you to be responsive and each baby is different. Don’t place expectations on your baby that s/he can’t meet just because another baby does. It will be worth it in the end to love and nurture your baby, just as s/he is.
***
If you are in need of individualized parenting help, I offer services via email, Skype, and phone on a variety of parenting topics. You can find out more here.







I’ve actually read her book that my friend recommended to me, I think it was the contented baby one, and she tells you when to drink water too, as part of her schedule. As if we all operate on an “I drink water at 7:23pm” kind of way!
The one thing I took away from it that was actually beneficial, was to give the baby some diaper free time. Totally enjoyable. The rest was pretty ridiculous.
First, to correct a couple of points: Gina Ford has never advocated that you should *only* feed a baby at the scheduled times. She advises feeding at the scheduled times, but also feeding if they’re hungry at any other time. And an earlier version of ‘The Contented Little Baby Book’, which I think predated the official advice about keeping babies in the same room, did advise putting babies down for naps in their own room, but later works of hers have changed that advice and now advise keeping baby in the same room as the parents to prevent SIDS. (I don’t know why she didn’t issue a rebuttal – since the Mail is a known rag and the article in question was referring to an argument with Clegg to which she’d already issued a response elsewhere, my guess is that she probably decided it wasn’t even worth reading it. If so, good for her.)
Also, I have to say that I think it’s downright silly to claim that waking a baby is going to make the baby dangerously sleep-deprived. *Keeping* a baby awake for extended periods when they want to go to sleep might well do so, but that’s the opposite of what Ford advises.
If you wake prior to when you are ready to be awake, are you not ready to go back to sleep and are being kept up?
Yes, but that’s hardly on the same level as being sleep-deprived to a dangerous degree! I think that’s a real stretch.
I’m also wondering – has research actually *shown* a link between SIDS and keeping a baby awake to the point of overtiredness? Or is that just a theory? I couldn’t find any studies on this on Pubmed. I’m open to the possibility that I may have missed something, but if the most we have on this is a *theory* that overtiredness *might* increase SIDS risk, then it’s even more of a stretch to get from that to the implication that you shouldn’t wake your baby up at a particular time for fear of putting him/her at risk of SIDS. Honestly – that’s exactly the sort of thing that would have freaked me out if I’d read it as a new parent, and I would have been forever wondering if it was wrong to pick up my baby in order to go out in case that woke him up and increased his SIDS risk, or to wake him for feeding prior to a long car drive… it would have been yet another thing to make me a nervous wreck.
I can certainly agree that it’s not good to get too hung up on waking your baby at a particular time, and that that should be very much a ‘horses for courses’ rule. (Which, by the way, is exactly how Gina Ford says she meant her schedules to be used, although I agree that that approach doesn’t really come across in her books.) But I think there’s a difference between ‘look, there’s no need to treat that rule as gospel, you can end up with a routine regardless of whether or not you do that so figure out whether it’s working for you’, and coming up with a contrived reason, on very flimsy evidence and logic, why waking babies must be a Bad Idea. That’s just another way of making a one-size-fits-all rule.
“I’m also wondering – has research actually *shown* a link between SIDS and keeping a baby awake to the point of overtiredness?”
Topkek, let’s research this until enough babies die to form a definite scientific connection! Science cannot function and therefore the world will crumble if there are not enough death and blood. Geez, just how American can someone be?
I think it’s also important to distinguish between ‘crying down’ and sleep training. (You may of course disapprove of both of them, but it’s important to recognise that they’re not the same thing.)
Some babies simply seem to be kept awake by attempts to comfort them to sleep and to need a few minutes of crying by themselves in order to get to sleep. ‘Crying down’ is the process of giving those babies those few minutes alone crying that they need. The difference between that and sleep training is that sleep training is the process of teaching a baby how to get to sleep by themselves, whereas a baby who needs ‘crying down’ time already knows how to get to sleep by themselves and in fact finds that easier than being put to sleep; they just need that few minutes of crying down time in order to do it.
I can vouch for this one from personal experience, as my daughter was like this. I can’t tell you how long I spent trying to settle her to sleep without success; depending on how tired she was, she would either cheerfully play with me with no sign of wanting to go to sleep, or she would cry and keep crying while I tried to settle her. The only reason I discovered what she actually needed at bedtime was because she’s my second child and so, in practice, I *had* to leave her sometimes. What I found was that, when I left her alone, she would always follow the same pattern; a couple of indignant wails, about seven or eight minutes of the kind of one-note crying babies do when they’re more fed up than acutely distressed, and then silence. If I went back in to comfort her at any time during that, she would immediately escalate back to the indignant wails and take much longer to settle down. Same pattern. Over and over again. I’ve heard many similar stories from parents (there is an excellent post about this at http://askmoxie.org/blog/2011/01/tension-decreasers.html). This is simply what some babies need to get to sleep.
Now, of course, the big problem with Gina’s rule is that she talks as though this applies to *all* babies, and that’s just as bad (actually, worse, since babies who need ‘crying down’ time seem to be a minority). But you’re talking as though it doesn’t apply to any babies and every baby ought to be comforted to sleep as a universal rule. From my own experience, I can tell you that this isn’t so, and that responsiveness to my daughter and her needs *did* involve leaving her for ‘crying down’ time. I think that’s an important point to bear in mind.
Dr Sarah, I totally agree with you regarding “crying down”, I was visiting a friend with a wee daughter (ten months old) and on putting her down for her morning nap, the wee babe proceeded to wail (not in a frantic or upset way) for two minutes then conk out for a 1.5 hour sleep! Turns out, it was just her way of winding down and something she’d always done!
With regards to waking a baby at 7am every morning, it’s not something I’d do with a newborn or a very young baby but it certainly helped us when my six month old was struggling with night sleep. We found that initiating a consistent wakeup time really helped with naps and bedtime because she thrives on routine and it meant that she was in bed at a reasonable hour each day.
Dr Sarah, just out of curiosity, and it’s not to try to disrepute you but what is your doctorate in, as if it’s in any paediatrics or such like than that’s great but if your Dr title has nothing to with the above topic, then people may see the Dr title and wrongly take your assume that you are qualified in this area. If you are then that’s great.
Ultimately it’s down to down to parents some prefer routines some prefer a more holistic approach, I tried both (I have 3 kids) in my experience I found the holistic approach worked so much better and that the routines approach has, like thee author of this stated, affected my relationship with my oldest child and her temperament now.
I have studied paediatric medicine, and also holistic and alternative therapies and have studied a lot of research into behaviours of children and adults.
Dear Tracy,
I got sucked into your article when peering over my wife’s shoulder and I think that you are doing great work going up against this Gina Ford woman. I have heard allot of her nonsense from other parents and find her methods antiquated, lazy, selfish and detached from all that is parenting, not to mention robotic. I admire your down to earth, natural and logical ways and hope that you continue to set Gina Ford straight. Definitely a fan.
Why thank you!! It’s always nice when you can manage to catch someone’s attention unintentionally 😉
The rule that really struck me was: don’t make eye contact with your baby. The only other situation I can think of that I’ve ever heard such a rule is in the midst of the Spanish Inquisition. It was one of the rules for torturing women. Don’t look into their eyes or they’ll bewitch you. In other words, if you don’t look into their eyes sympathy and empathy will not get the better of you and you’ll be able to keep torturing them. Scary sort of rule to apply to a baby….
Hello, thanks so much for this information, I’m a FTM and have been “winging it”, and by a happy coincidence, have been following much of what you suggest. Yay! My question is regarding naps. I have been in a fairly dark room with a sound machine for her naps (5 months old). Often I sleep with her, as she sleeps so much better/longer with a nap companion. How can I implement on the go naps? She hates her car seat half of the time, and I feel like we do a form of CIO when we have to go anywhere and it breaks my heart, but what do you do?? So, napping in the car is out. Any suggestions or recommend articles/books/etc…??
What about babywearing?