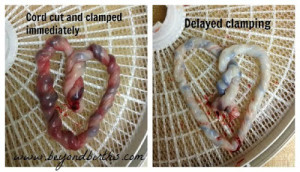
 In today’s modern birthing picture, you finish birthing your baby and the doctor immediately clamps the cord and you wait to expel the placenta before cutting. However, this isn’t actually the norm around the world (though notably there is variability worldwide in clamping practices currently). Often, mothers engage in what is, in our culture, called “delayed cord clamping” and there’s reason to believe we ought to be changing our norms as well…
In today’s modern birthing picture, you finish birthing your baby and the doctor immediately clamps the cord and you wait to expel the placenta before cutting. However, this isn’t actually the norm around the world (though notably there is variability worldwide in clamping practices currently). Often, mothers engage in what is, in our culture, called “delayed cord clamping” and there’s reason to believe we ought to be changing our norms as well…
What is “Delayed” Cord Clamping? (And why it is really not “delayed”.)
You may hear someone speak of “delayed” cord clamping which refers to clamping the umbilical cord after the cord has stopped pulsing or after a period of time of 2-3 minutes (typically). This is in contrast to what has become more common which is early cord clamping, or the clamping of the umbilical cord immediately after birth without waiting for the cord to stop pulsing.
The reason it’s not “delayed” is that waiting for the cord to stop pulsing is actually the most biologically and evolutionarily normal thing to do. Women never used to clamp early, but rather simply let nature take its course with the cord being clamped and cut after a period of time.
Why did we Start Early Cord Clamping?
A few decades ago, doctors decided that early cord clamping would be beneficial in certain ways as people believed that babies were receiving too much blood (yes, I’m not kidding). It has been argued that too much blood results in jaundice
[1], respiratory problems[2], and polycythemia[3] (polycythemia is a blood disorder in which bone marrow makes too many red blood cells). It was also thought to prevent post-partum haemorrhage in women[4], the leading cause of maternal death during pregnancy worldwide. And so it became more and more common for hospitals to encourage early cord clamping such that it has now become the norm, so much so that people do believe there is some type of “delay” when it’s not clamped immediately.
How does cord clamping relate to these conditions? Well, based on the Cochrane Collaboration report[5], we know that early cord clamping does not influence maternal haemorrhage at all, both for regular and severe haemorrhage. We also know that there are no effects on respiratory distress, clinical or symptomatic polycythaemia, and clinical jaundice. The only area that seems to hold up is that, looking at data over five trials, there was a decreased risk of jaundice requiring phototherapy in the early cord clamping group. (It is worth noting that another meta-analysis did not find the same decreased risk of jaundice requiring phototherapy associated with early cord clamping and instead found no difference in the two clamping practices[6].)
What are the Benefits to Normal or Optimal Cord Clamping?
The very first benefit is that your baby can receive up to an additional 30% of blood and up to 60% more red blood cells during this period[7][8]. This allows organs to receive more oxygen which improves overall health. The body also receives vital stem cells which aid in the reparation and regeneration if there are problems (this is why if you choose to harvest your child’s cord blood you must clamp early; you can read more on this here).
The most robust finding with respect to normal or optimal cord clamping is to do with iron. As many parents know, the risk of anemia in children is quite high in our society and as such parents on consistently pushed to supplement with iron-fortified foods, especially when breastfeeding. However, the other option for those who know of it well-enough ahead of time, is to not early cord clamp. In terms of the research, one meta-analysis found higher ferritin concentration, stored iron, and reduction of risk for anemia for those infants whose cored was clamped later[6]. This was also replicated in the Cochrane report on cord clamping[5]. Notably, these results hold at 2 months and 6 months, suggesting it is not just a short-term effect. In one specific study, it was found that clamping the cord after 2 minutes resulted in an increase of iron stores at 6 months of 27-47mg[9].
One group of infants who almost inevitably are early clamped are pre-term infants. The reason has always been the rush to get them into care (e.g., oxygen, blood transfusions, heat, etc.); however, research has started to show that there are benefits to waiting even just 30 seconds to clamp in pre-term infants. Preterm infants (average of 28 weeks) in a controlled trial of cord clamping after a 30-45 seconds wait versus immediately were found to have a significantly lower risk of intraventricular haemorrhage and late-onset sepsis[8].
Another randomized trial of preterm infants between 27 and 33 weeks found that those whose cord was clamped after 30 seconds (as opposed to immediately) showed immediate effects including higher packed cell volume, lower concentration of red blood cells transfused, and lower supplemented oxygen time overall of 2 days compared to 5 days (when looked at just the infants who had to be ventilated it was 3 days compared to an average of 10 days)[10]. Furthermore, these effects were linked with other elements of longer-term health, suggesting even just a short delay can have profound clinical implications for vulnerable neonates.
Additional Things to Consider
Despite the evidence favouring normal cord clamping, particularly for iron stores, there seems to be some misconceptions about how beneficial it is on other areas. I have read people claim it helps Vitamin K stores, which we know it does not. In fact, unless mom is injected with vitamin K just prior to delivery, vitamin K is not found in the babies’ cord plasma and is suggestive of the fact that vitamin K does not cross the placenta readily or the fetal uptake is very low[11]. It has also been suggested that it can help prevent haemorrhaging in full-term neonates. There is no research suggesting this is the case (though it does reduce the risk of intraventricular haemorrhage in preterm neonates, as mentioned above); however, the larger supply of blood does mean that some blood loss may be relatively safer due to a larger supply of blood to begin with but I have no research to suggest any differences in haemorrhage rates based on the timing of cord clamping in full-term neonates.
Finally, it is worth mentioning that the aspects of delivery can influence the degree to which waiting to clamp can be beneficial. For example, c-sections do not often present with the same level of increased blood flow between the cord and the infant[12], suggesting that either timing may need to be longer in these cases or that we may not see the same results. Furthermore, the angle at which the infant is held while the cord continues to pulse will affect how much blood is transferred to the infant in a given time[7]. For example, raising the infant 30-60 cm will slow the amount of blood delivered to the infant while lowering the infant can almost triple the speed at which blood is transferred.
Conclusion
Waiting 2-3 minutes, or until the cord stops pulsing, in full-term neonates or 30-45 seconds in preterm neonates can offer significant benefits to baby both short and long-term. Though there is perhaps an increased risk of jaundice (depending on which reviews you look at), the overall benefits of waiting to clamp seem quite clear, especially today when more and more babies are iron-deficient. For preterm babies the benefits are even greater, with clinical outcomes showing that waiting even that brief period to be immensely valuable to their well-being. If you are pregnant or thinking of getting pregnant, you should speak to your care provider (doctor or midwife) about this practice. Though it hopefully becomes the norm again in modern birthing practices, in the interim it’s up to you to make sure your rights are respected for it.
[Image Credit: Beyond Births]
[1] Blackburn S. Hyperbilirubinemia and neonatal jaundice. Neonatal Netw 1995; 14: 15-25.
[2] Oh W, Wallgren G, Hanson J, Lind J. The effects of placental transfusion on respiratory mechanics of normal term newborn infants. Pediatrics 1967; 40: 6-12.
[3] Oh W. Neonatal polycythemia and hyperviscosity. Pediatr Clin North Am 1986; 33: 523-532.
[4] McDonald S. Physiology and management of the third stage of labour. In: Fraser D, Cooper M editor(s). Myles textbook for mid-wives. 14th Edition. Edinburgh: Churchill Livingstone, 2003.
[5] McDonald SJ, Middleton P. Effect of timing of umbilical cord clamping of term infants on maternal and neonatal outcomes. Cochrane Database of Systematic Reviews 2008, Issue 2. Art No: CD004074.
[6] Hutton EK, Hassan ES. Late vs early clamping of the umbilical cord in full-term neonates. Journal of the American Medical Association 2007; 297: 1241-52.
[7] Mercer JS. Current best evidence: a review of the literature on umbilical cord clamping. Journal of Midwifery and Women’s Health 2001; 46: 402-14.
[8] Mercer JS, Vohr BR, McGrath MM, Padbury JF, Wallach M, Oh W. Delayed cord clamping in very preterm infants reduces the incidence of intraventricualr haemorrhage and late-onset sepsis: a randomized, controlled trial. Pediatrics 2006; 117: 1235-42.
[9] Chaparro CM, Neufeld LM, Alavez GT, Cedillo REL, Dewey KG. Effect of timing of umbilical cord clamping on iron status in Mexican infants: a randomized controlled trial. The Lancet 2006; 367: 1997-2004.
[10] Kinmond S, Aitchison TC, Holland BM, Jones JG, Turner TL, Wardrop CAJ. Umbilical cord clamping and preterm infants: a randomized trial. BMJ 1993; 306: 172-5.
[11] Shearer MJ, Barkhan P, Rahim S, Stimmler L. Plasma vitamin K1 in mothers and their newborn babies. The Lancet 1982; 320: 460-3.
[12] Narenda A, Beckett C, Aitchinson T, Kyle E, Coutis T, Turner T, et al. Is it possible to promote placental transfusion at preterm delivery? [abstract]. Pediatr Res 1998; 44: 453.






My friend and I were just having a discussion about this! She said that her midwife told her delayed cord clamping was a bad idea and they wouldn’t do it because of the altitude here (5,000 ft) in Colorado. Have you heard of this? What difference would altitude make? It sounds like a great idea to me and I’d like to delay cord clamping with my next, so thanks for this article! 🙂
I have read about a lot of factors but never seen anything about altitude, though the effect of altitude on blood would actually promote a benefit of cord clamping. In high altitudes we get LESS oxygen in the blood and in organs, so early clamping would mean even less oxygen for babes whereas delayed clamping would allow more oxygen to flow to the baby and organs. But perhaps there’s something I’m missing??? I’d have her ask the midwife WHY it’s a bad idea!!
OK, I’ve read some more and heard of some midwives and doctors using this excuse, but heard no one’s seen evidence of it (i.e., their doctors and midwives can’t provide evidence) and that there are many doctors and midwives in CO who regularly delay cord clamping. So it seems it’s more something the midwife doesn’t want to do??
That doesn’t make any sense. I live in Colorado and I know that blood carries oxygen, sooooo having more blood would mean MORE oxygen. Makes no sense and is probably something they made up. Medical Professionals, in my experience, tend to lie a lot to get you to do what is easier for them. I would think getting enough blood back from your placenta would increase blood oxygen levels simply from the virtue of having more blood?
In regards to the jaundice issue: based on what you came across, would you say there was any argument for early clamping in 2nd/3rd children if the first was quite jaundiced (and parents/immediate family were very jaundiced at birth? Or is the increased risk for jaundice even for families known to have jaundice problems not significant enough to disregard the other benefits? (Did that question even make sense, lol?)
The question totally made sense and I didn’t come across anything on that. I would talk to your care provider about that issue, I’m not sure if the risk is there regardless or if it would be worse with later clamping.
lol, unfortunately, my care provider (the only group covered) is a knob. We asked for delayed clamping with the first and she agreed, but when it came to it, she refused to hand him to me before clamping because “all the blood will rush out of his body into the placenta if he’s held higher than the placenta” (which hadn’t been delivered yet). Have you considered writing a short piece on placenta birthing practices? The pitocin made me shake so hard I couldn’t hold my own cup, but then they gave me a huge injection to make me birth the placenta faster (and quite forcefully). I’m convinced that’s one of the reasons I bled so much and needed a transfusion postpartum.
It actually is on my list of things to write on (sadly a very long list that keeps growing faster than I can keep up with it)!!! But really, your care provider sounds like an idiot. My goodness – glad you got out alive 🙂
I read in one of my pregnancy books recently that “delayed” cord clamping can also be beneficial in the case of a mother with Rh- blood with a baby who may have Rh+ blood. The book claimed that as the placenta starts to detach from the uterine wall, blood vessels may break; if the cord is clamped early, the placenta will have more fetal blood left inside it, creating a significantly higher chance of the mother getting the Rh+ blood in her bloodstream and potentially creating antibodies against it. However, by clamping later, more of the fetal blood will be in the baby (instead of the placenta), lessening this risk. Do you know anything about this?
I haven’t, but am fascinated by it (as an Rh- mom, though married to a same-blooded man so our daughter’s also Rh-). I don’t know if there’s even enough research on it to know if that’s a thing, but something I will definitely look into!! Thank you 🙂
I attended a course called calmbirth (australia) before giving birth which encouraged delayed clamping and refusing syntoxin injection. Both were denied when I requested these during labour, as its unconventional. I think health professionals should be updated with current findings and respect the mothers giving birth if evidence supports their wishes for a more natural approach to birth. I was also encourage to push during labour when I have no urge to but that’s a different story.
We decided to bank our first baby’s cord blood, and we’re not sure what to do about the second one. Do you think the benefits of delaying cord-clamping outweigh the benefits of privately banking cord blood?
I think it’s a personal decision. For me, yes, the benefits of delayed clamping outweigh private banking. However, some people have mentioned that their caregivers will try both which may be the best of both worlds if you’re interested… just ask your care provider!
[…] Why “Delayed” Cord Clamping Should Be the Norm … – My friend and I were just having a discussion about this! She said that her midwife told her delayed cord clamping was a bad idea and they wouldn’t do it because of … […]
[…] red because we delayed cord clamping until the umbilical cord had completely stopped pumping blood (https://gku.flm.mybluehost.me/evolutionaryparenting.com/delayed-cord-clamping/). Kevin explained this to her–that Apollo had a higher volume of blood and therefore a higher […]