
One of the more common problems with bedsharing in our modern, Western culture is that few people actually intend on doing so and in turn when the majority end up bedsharing in order to get some sleep, they haven’t actually made the bed in a safe way for an infant. I have thoroughly reviewed the research on bedsharing and on its own it isn’t a risk; however, there are social factors that interact that increase the risk (the syndemics approach taken by Drs. Cecilia Tomori and Melissa Bartek highlighted various social factors that have been ignored yet play the key role in SIDS and suffocation deaths) and also environmental risks in the bed itself. It is the latter issue that I hope to cover here to help families be as safe as they can.
This means this is really for anyone who is pregnant or who has a newborn that they still believe will never enter your bed (or for those who have already done some unexpected bedsharing and aren’t sure where to turn for safety).
First off, let me say congratulations. New babies can be terrifying but oh-so-exciting. I imagine you’re getting lots of advice from well-meaning others, especially of the kind surrounding how tire you will be and how to cope with massive sleep deprivation. What many people won’t tell you is that the way humans have coped with this sleep deprivation for most of human history is to try and avoid it by sleeping with baby as much and as safely as possible.
You see, your baby expects to be close to you at all times. This keeps them feeling safe and also facilitates breastfeeding (whether you breastfeed or not, your baby expects breastfeeding at a biological level and thus proximity is essential) and so the human norm for sleep is what has been coined “breastsleeping” by Drs. James McKenna and Lee Gettler. Some babies will do okay being in a cot next to their parents bed*, but many babies will tolerate this about as well as an ice cold bath. This means babies will cry and cry until they are picked up and soothed by a parent, only to repeat the process after going back down. Clearly this means there are a lot of tired nights ahead of you.
*I only mention sleeping in a cot next to you as Safe Sleep Guidelines and research show us that babies being in their own room increases the risk of SIDS two-fold and thus is not recommended at all.
In many cases, babies will be able to connect cycles a little easier and give Mom (yes, Mom, we’ll get to that below) some much-needed sleep. When talking about this, I always share this image that was sent to me years ago from a Mom who had not been bedsharing and then one day decided she had to:
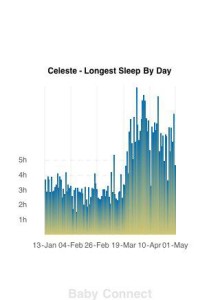
Photo Credit: Celeste
So there is good reason why many parents who think bedsharing is dangerous and don’t plan on doing it end up bedsharing and unfortunately end up bedsharing in the very same dangerous situations they first thought of when considering bedsharing. The question then is how are you going to avoid this trap?
PART ONE: LOOK AT YOUR BED
The bed is often the dangerous element for a baby. Our modern, adult beds can be soft with lots of pillows and fluffy duvets (especially if baby is born in winter), all of which pose a serious hazard to your baby’s well-being. The following are what you want to look for now so you can make sure that things are safe in your bed. Update: I have provided age ranges, but they are estimates only as we don’t actually have good upper age limit research on this so really you can continue this for as long as you are comfortable. For the most part, SIDS risk is negligible after a year and so that is the general limit, but research finds that most non-suffocation risk factors decrease after 4 months of age.
- Firm mattress. Any soft mattress is NOT safe as your baby cannot roll and if he or she were to end up face into the mattress, suffocation could follow. One way to tell if your mattress is firm enough is to lay with baby on the bed and see how much you cause baby to move towards you. It’s not enough just to place baby on the bed to see what happens as often the problem is we sink in and this causes baby to roll towards us and get stuck against the mattress. A firm mattress will not cause such a situation. Age range: Minimum 1 year for firm, but a soft mattress should not be used until significantly older.
- No added pillows. Yes, you will likely use a pillow (the smaller, the better), but you do not want a bed filled with pillows or large pillows that extend far around you that could block baby’s face. Age range: Most recommendations are not for at least the first year though many kids don’t even want pillows until closer to 2-3 years of age.
- No duvets. Duvets are too big and fluffy and a suffocation hazard. They are also incredibly hot should a baby end up under them (we’ll discuss this). Age range: 18 months or over.
- Nothing else. No stuffed animals (yes, I know we’re adults), no extra blankets, nothing. Age range: 18 months or over.
- Proximity to the ground. Babies can fall off beds so you being close to the ground is much better than being high up. This is especially true as bumpers or bed rails are not safe for babies and so you cannot use them to keep babe from falling out as they present their own suffocation risk. You do not want your mattress directly on the ground as this can be dangerous due to any trapped moisture leading to mould growth; however, you can just put some wood slats with space under the mattress and this would serve to allow air flow and keep the mattress safe. Age range: 2 years when it is safe to add a bed rail.
- Position relative to the wall. There is some confusion over this because some places speak about the bed being safe when flush up against the wall, some say that’s dangerous. From what I can gather, the danger is when people use a bed frame for the mattress as this adds extra space between the mattress and the wall. When a bed frame is used, the bed may be flush against the wall, but the mattress isn’t. It is the mattress that needs to be flush so there is no space for baby to end up with his or her head part way against the wall or mattress and unable to breathe. However, if you’re low, there’s no reason to fear having the bed away from the walls as falling out of a small bed won’t be the end of the world. Age range: 2 years when it’s safe to add a bed rail.
PART TWO: LOOK AT YOUR SITUATION
The other part that can be dangerous is when it’s the parent’s behaviours or situation that puts their baby at risk. There are certain things that seem to increase the risk of SIDS and suffocation, especially in conjunction with bedsharing. If you do not meet any of these criteria, please know that you can bedshare with minimal risk (minimal because there is always risk in everything). Update: I have also added age ranges here, though again there is little research on the upper end with most people considering the end of the SIDS risk (at 1 year) to be the final say.
- Formula feeding. This is actually somewhat debatable based on the very minimal data we have, but as the evolutionary norm is breastfeeding and there is some evidence that formula feeding moms position their babies in a more dangerous way, this is something to consider. Age range: Unknown and it’s unclear if the risk is actually greater than the risk of formula feeding to SIDS. Regardless, 4 months may be a good age given the research on the reduction of risk of bedsharing at that age.
- If you are on any medication that makes you drowsy, it is imperative you do not bedshare with your baby. Age range: Until your child is old enough and strong enough to move you if you roll on them if you are unable to wake.
- There is some evidence that being obese can mean a higher risk of danger for baby. Age range: Again, unclear, but likely once baby can safely move, so 6-8 months, but this is simply a guess.
- Smoking is even worse than drugs and alcohol (seriously) in the research. For whatever reason, just having the smell of smoke on you while bedsharing is a massive risk factor for SIDS (in some studies, the biggest risk factor). Age range: 1 year or older as this is one of the greatest risk factors for SIDS so you want to go as long as possible.
- Another child in the bed. You do not want a baby sleeping next to another child as they do not wake or have the type of spatial awareness you will. This means that you want an adult (i.e., you) between any two children in the same bed. Age range: Until your child is strong enough to move away from a sibling.
PART THREE: TEMPORARY FACTORS
Here is where we want to talk about things that may affect your ability to bedshare safely but are easily modifiable and if not, you should consider. This means that these are elements that you will have to remember so that on those hard nights you can safely bedshare, but if you can’t modify these things, you should try to avoid bedsharing until you can safely address them. Update: Again, have added age ranges and again, they are not concrete as the research isn’t concrete.
- Drugs and alcohol. These things impair your ability to respond to your child and thus should not be used excessively or too close to bedtime (that glass of wine at lunch or even dinner isn’t the killer). If you have taken part, take care to place baby in safe space for that particular night. Age range: Until your child is strong enough to move you should you be unable to move if on top of them.
- Long hair. If you have long hair it is best to tie it back when sleeping with babe. This can mean getting in that habit or having an elastic next to the bed in case you do bring baby to sleep with you on a given night. Age range: 8-12 months, when babies can safely move away from the hair.
- Jewelry. Remove any long jewelry that baby could get caught up in or choke on should baby get it into his or her mouth. Age range: Never, they are a choking hazard and if there is a risk of them coming off in bed, they should not be worn to bed.
WAIT! SOMETHING DOESN’T WORK FOR ME – NOW WHAT?
What if you read these and something here doesn’t work for you? Here is where we can explore alternatives now so that you are prepared and can avoid the issue of unsafe bedsharing when/if the time comes.
If the bed is the issue…
- You can buy a single or double mattress that is firm and place it down in another room and set it up safely to use when you feel the need to sleep with baby close by for the night.
- You can look at using a side-car cot or making your cot a side-car one so baby is close and you can touch him/her during the night without being on your bed.
If your situation is the issue…
- If it’s formula, you can do research on positioning to ensure you follow safe position of babies when bedsharing. (Briefly baby should not be at eye-level, but at breastlevel and not under any blankets, but in their own sleep sack, if needed; really imagine if you were breastfeeding where baby would be.)
- If it’s medication, you can ask your doctor if there is another medication you can take that would not cause drowsiness.
- If it’s smoking, consider quitting now or at least know that bringing baby to bed is a really, really, really bad idea. Look into room-sharing (there is no additional risk there) and know that you may be tired. I would make sure you have appropriate daytime support to help with your tiredness so you don’t feel pressured to bring baby to bed for some sleep. (Note this may be very important as some research suggests babies whose moms smoke are fussier as well and so you may be even more prone to want to bring baby to bed.)
- If it’s obesity, you can talk to your doctor or again consider the side-car cot as a safe alternative.
- If it’s another child, you can set it up so both kids are in bed, or you may have one partner (if there are two of you) sleep with the other child for a spell.
If temporary factors are the issue…
- If it’s drugs and alcohol, just avoid and try to get help if you don’t feel you can cut back on your own.
- If it’s hair, as mentioned, keep an elastic next to the bed to put your hair back.
- If it’s jewelry, take it off and if you can’t, you can try to tie it up as well.






Hi Tracy, could you please offer some pointers as to the age range this (or some of it) applies to? I’m guessing there must be a threshold yet normally it’s never included or discussed. Especially since some of the concerns (e.g., small space between the mattress and the wall that occurs if bed is flush to the wall) must surely be more applicable to newborns than to toddlers? Thank you!
Great point Sara – I’m heading out of town but when I return I’ll try and remember to update this. If I don’t by the end of the month, can you remind me?
Hi Tracey. I was just about to post the same question. There’s a use of the word baby with no especification of age. I would think some of the risks change when baby is say 7/8 month old? Or when baby reaches certain milestones? What’s the research out there saying if you don’t mind sharing? I always wonder this in regards to SUDI as well…
Hi Tracey!
Just wants to echo the same question as above. Any thoughts to the age differences of babies and if certain guidelines fluctuate some?
Thanks!
Thank you for the reminder – I have now updated it 🙂
I’m confused as to the age ranges. A range is usually from one number to another, but you only have one number for most of these. Do you mean these are minimum ages, before which you should just not?
Exactly 🙂
Hi! It says minimum 1 year for a firm mattress. What would you use before a firm mattress then?