 There’s news about an article making the rounds regarding the risk of homebirth. Notably, two individuals have written an article for the Journal of Medical Ethics
There’s news about an article making the rounds regarding the risk of homebirth. Notably, two individuals have written an article for the Journal of Medical Ethics
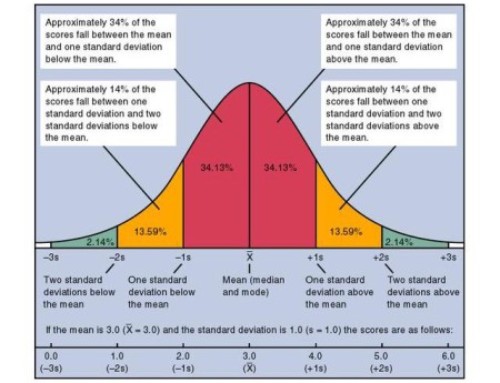
The question becomes, what evidence did they use to make this decision? Well, they very rightfully note that there is virtually no research on long-term disabilities related to location of planned birth. This is a huge flaw in the system and one every country should look into. However, I say “virtually” because all we have to go on is one large-scale study out of the UK[2] which did examine long-term outcomes. Now, because the base rate is so low, they lumped all long-term outcomes together because they didn’t have the power to detect any one individually. This is a flaw because it means less severe outcomes are mixed with more severe, but this is a regular problem when baserates are low. What did they find? No difference in long-term outcomes for planned home versus planned hospital births for multiparous women. In the UK. This is obviously limited research and not something we can take to heart as being definitive, but it suggests that in a system such as the UK, planned home birth may not have any increased risk for later outcomes. The authors, however, argue the potentials of what could go wrong because of delayed transport without any data to back up that the current guidelines about transfer times and homebirth in many countries are flawed.
Now what of death? Well, these authors focus exclusively on US data[3] (and a supplement that I have to take their word for because apparently it’s impossible to find even online, though the same authors have written up US data suggesting a higher risk to homebirth[4]) to suggest that homebirth is inherently less safe (and use the infamous Wax et al. study[5] which is considered a gong show at best from a methodological and statistical point of view). They don’t even include any references to the large-scale studies in Canada[6] and the Netherlands[7] that has found no increased risk for homebirth versus hospital birth and one US study looking at an integrated system (like those in Canada and the Netherlands) found the same outcome[8] (nudge, nudge, USA). The one study they included to try and argue that travel time matters even in highly integrated areas was based in the Netherlands and looked at travel time for all births (not home versus hospital) and was based on travel time of 20 minutes or less versus more than 20 minutes[9]. Travel time greater than 20 minutes was associated with greater death, regardless of planned location as this included just traveling to the hospital at the onset of labour. Given this is the time frame suggested in Canada too for a homebirth, it seems that it’s based on some evidence.
This is where my pet peeve comes in: When you’re looking at either mortality or morbidity from birth, you’re looking at an event that will be categorized by the health care system in which one lives. How a health care event unfolds is therefore going to be highly dependent upon the system in which it resides. As ethicists, I would sincerely hope that these individuals were aware of how ludicrous it is to take US data and use it to make recommendations for the rest of the world, especially when we have large-scale data from other countries that counter US data because of different health care systems. Furthermore, when you use data from one country with a health care system different from the rest and you try to demonize homebirth and the women who choose it (borderline suggesting it is immoral and should be illegal), you have a lot of explaining to do.
The authors state, “What we have argued is that a neglected ethically relevant outcome is serious avoidable, foreseeable disability to a future child.” Except later when they have to admit, “We have argued that in most situations the risk of disability may be elevated and unjustified.” (Emphasis mine.) In short, they don’t have any evidence this is the case, but assume it might be. What evidence they have suggests that there may be concerns dependent upon how far people live from the hospital (why many care providers in countries with an integrated health care system have distance from hospital discussions with women and their families), and they are right to suggest more research into it. What they cannot do is make conclusions in the manner they have from the evidence they have.
They also pull out the “one child harmed is too many” while ignoring the risks that may be present in a hospital (though they do give lip service to the “possibility” that hospitals can have risks too), playing it off as if only homebirth could be associated with negative outcomes. I actually couldn’t help but snort when I read, “[P]rofessionals should not support planned homebirth when there are safe and compassionate hospital-based alternatives.” I don’t doubt there are safe and compassionate hospitals out there or even compassionate doctors in hospitals that generally aren’t, but when a large portion of women are looking for homebirth because their hospital experiences were the antithesis of compassionate, these ethicists need to be looking at what they are suggesting.
Women and their families deserve to be given every bit of information they can, but that information should be specific to their health care system, their hospital, and their midwife or doctor or whoever they have providing support. Telling a woman in Canada that homebirth is riskier because it is in the USA isn’t true and certainly isn’t sound science.
[Image Credit: Unknown]




[…] debates about home birth you probably read some of the news stories that said that having a home birth is like driving in a car without a seatbelt. The pundits spreading those myths have their own biases. I find it ironic that mainstream medical […]
[…] is considered a pet peeve by many. Other driving-related pet peeves include drivers who speed up to keep others from […]
I couldn’t agree more. It’s one thing for people to express their personal opinion, it’s another for them to express that opinion as if it is scientifically proven fact! And that that fact works across every country and every different health care system.
I have work as an out of hospital medical professional for 20 years in the UK. I have been privileged to be involved in the births of many new lives, 7 of which were in the families own homes (1 of which was a breech birth, was one of the scariest moments of my life and I wouldn’t recommend doing at home) and from my experience home births tend to be calmer and less stressful for mother and baby. Looking at this logically, surely a less stressful and calmer birth, whether at home or in hospital, must be better for mother and child, both in the short term and long. So perhaps we should be doing more studies to improve the quality of the location rather than the location itself.
My wife and I are about to become parents ourselves for the first time and there was no hesitation from either of us, it’s home birth! Here in the UK there is a lot of emphasis on ‘centralising care’. This means that if we had a midwife lead birth in hospital we would have to go to a maternity unit that is actually further away from the main hospital that does consultant lead births. So if anything went wrong we would have a longer, more painful and distressing journey than if we stay at home.
It’s amazing how fast the “one child harmed is too many” argument comes out when discussing natural methods, but when it comes to prescription drugs or routine hospital procedures, suddenly massive side effects and a certain rate of casualty is the norm.