By Helen Ball, BSc, MA, PhD, Professor of Anthropology, Durham University
This review examines the issue of babies sleeping with their parents. Beginning with an anthropological perspective, the biological underpinnings of parent-baby sleep contact are explored, as are cross-cultural practices. The relationship between baby sleeping and feeding practices in the UK is considered along with the safety aspects of bed-sharing.
Introduction
This review considers babies’ sleep location at night, specifically parent-infant bed-sharing and/or co-sleeping. This is a baby care issue caught between two public health objectives, both aimed at preserving infant health and well-being – one being breastfeeding promotion, the other prevention of accidental death and SIDS
 Co-sleeping as an evolutionary baby care practice
Co-sleeping as an evolutionary baby care practice
When considering the needs of mothers and babies, the vantage point of anthropology provides a novel perspective (in comparison with epidemiology or clinical practice, for instance) in illuminating the tensions regarding infant care. An anthropological examination begins by drawing comparisons in infant care across humans and other mammals. This comparative mammalian perspective helps to define three things: a) those traits of human infants that are common to all mammals; b) those that are shared only with our closest primate relatives; and c) those that are unique to the evolution of our species. The fundamental commonalities shared with other placental mammals involve the production of relatively well-developed live-born young who require postnatal maternal care involving lactation (the defining characteristic of the Mammalia) [1].
Length of gestation period and developmental state at birth varies among mammals with infants generally categorised into one of two types. Altricial infants are the least developed at birth; typically born in litters following a relatively short gestation period they are hairless, sightless and deaf. Such altricial infants are sequestered in nests for safety and warmth while they undergo a period of rapid growth and maturation. They are fed infrequently by mothers who produce milk that is high in fat and which takes an infant several hours to digest. In contrast, precocial infants are born singly or in pairs, and are well developed at birth with fur, sight, hearing, and limb co-ordination. Typical precocial infants can stand and walk within a short period after birth. Precocial* infants are therefore able to maintain close proximity with their mothers, suckling frequently and at will, while the milk they consume is relatively low in fat but high in calories (lactose) providing energy in a quickly digested form [2].
Among the primates (the order to which humans belong) monkey and ape infants fall into the precocial category – born following a relatively long gestation period with fur, vision, hearing, and the ability to cling to their mother from birth. Human infants then, conform by consequence of evolutionary relatedness to this precocial primate pattern, being born with hair, sight and hearing. Yet human infants also display what are known as ‘secondarily altricial’ characteristics – primarily lack of neuromuscular control – a consequence of the limits imposed on gestational brain development by the evolution of the human pelvis. Human infants are born with a brain that is only a quarter of its adult volume (compared to 50% for infant chimpanzees and gorillas) due to the constraints of a birth canal that has been modified to accommodate upright walking. Although displaying many precocial traits, therefore, human infants are dependent upon a caregiver for maintaining close proximity, and for the regulation of physiological functions such as temperature and breathing during the first few months of brain development [2] [3].
Human milk has a similar composition to that produced by other precocial primates, relatively low in fat and protein, but high in sugar (in the form of lactose) [4]. It is milk that is ‘designed’ for infants who suckle frequently and of their own volition day and night. Due to their inability to cling, however, human infants are dependent upon their mothers to ensure that proximity is maintained. Ethnographic data from societies around the world confirm that mothers in traditional human cultures are in contact with their infants 24 hours a day, carrying them strapped to their bodies by day, sleeping beside them at night [5], and feeding at will. Consideration of the human neonate from an evolutionary perspective throws the recent history of infant care in our own society into sharp relief.
‘…the modern Western custom of an independent childhood sleeping pattern is unique and exceedingly rare among contemporary and past world cultures’ [6].
Since the mid-1930s, prolonged and independent night-time sleep has been the hallmark of a ‘good baby’ in many Western societies; early infant independence is viewed as a developmental goal, and its achievement as a measure of effective parenting [7][8]. Yet for the majority of the world’s cultures, separation of an infant from its mother for sleep is considered abusive or neglectful treatment for which Westerners are criticised [9][10]. In US and UK households separate sleep locations for parents and infants are historically recent – less than two centuries ago mother-baby sleep contact was the norm with entire families sleeping together [11].
The importance of inter-individual contact on the physical and psychological development of infants was revealed in the mid-twentieth century by the experiments of Harlow and colleagues on monkeys separated from their mothers at birth [12]. Subsequent research on human and nonhuman primate infants has demonstrated that infants’ most fundamental physiological systems such as breathing, heart rate, sleep architecture, and thermoregulation are affected by the presence or absence of parental contact [13][14][15][16]. As a consequence of this research the past two decades (1989-2009) have witnessed a) a renewed recognition of the importance of contact and touch for babies in the context of improving breastfeeding initiation and duration [17]; b) an increased awareness of the role that close parental proximity and monitoring of babies plays in reducing SIDS and neglect [18][19]; and c) the impact of early mother-infant separation on long-term mental health [20] – all leading to a resurgence of interest in parent-infant contact, particularly sleep contact.
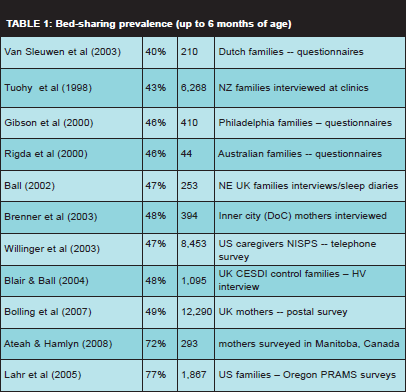 Given the well-recognised importance of close contact in establishing breastfeeding, and the need for frequent suckling, anthropologists consider that mother-infant sleep contact is a normal, species-typical, parenting behaviour for humans. Over the past 15 or so years, research into parent-infant sleep behaviour the UK, and around the world, has revealed that contrary to earlier assumptions [21], parent-baby sleep contact is a common baby care practice. Ball [22][23] reported that bed-sharing prevalence (ever sleeping with baby in the same bed) in the north-east of England was 47% among a sample of 253 families with 1 month old infants, dropping to 29% when the same babies were three months old. These figures were confirmed when Blair and Ball [24] compared the above study with data from the 1095 UK national CESDI study control families. Using the same definitions of bed-sharing at identical timepoints 48% of CESDI control families had slept with their infant during the first month, falling to 24% at three months. The establishment of a base-line bed-sharing prevalence of 47-48% among neonates has subsequently been replicated by epidemiological studies around the world (see Table 1) and further confirmed for the UK by the 2005 Infant Feeding Survey [25]. Both McCoy26 and Blair and Ball24 also calculated that 22% of infants were likely to bed-share on any given night in their 1st month of life. These figures indicate that parent-infant sleep contact is a common night-time infant care-strategy in a wide variety of western countries.
Given the well-recognised importance of close contact in establishing breastfeeding, and the need for frequent suckling, anthropologists consider that mother-infant sleep contact is a normal, species-typical, parenting behaviour for humans. Over the past 15 or so years, research into parent-infant sleep behaviour the UK, and around the world, has revealed that contrary to earlier assumptions [21], parent-baby sleep contact is a common baby care practice. Ball [22][23] reported that bed-sharing prevalence (ever sleeping with baby in the same bed) in the north-east of England was 47% among a sample of 253 families with 1 month old infants, dropping to 29% when the same babies were three months old. These figures were confirmed when Blair and Ball [24] compared the above study with data from the 1095 UK national CESDI study control families. Using the same definitions of bed-sharing at identical timepoints 48% of CESDI control families had slept with their infant during the first month, falling to 24% at three months. The establishment of a base-line bed-sharing prevalence of 47-48% among neonates has subsequently been replicated by epidemiological studies around the world (see Table 1) and further confirmed for the UK by the 2005 Infant Feeding Survey [25]. Both McCoy26 and Blair and Ball24 also calculated that 22% of infants were likely to bed-share on any given night in their 1st month of life. These figures indicate that parent-infant sleep contact is a common night-time infant care-strategy in a wide variety of western countries.
In one of the first studies examining bedsharing practice in the UK, Ball et al [27] discovered that although prospective parents did not anticipate sleeping with their newborn baby, by three months after birth, the majority of parents had done so. Mothers were more likely to sleep with their babies than fathers, and breastfeeding mothers particularly so. In a subsequent study Ball [23] reported that 72% of babies who were breastfed for a month or more were at least occasional bed-sharers compared to 38% of babies who had never breastfed. UK mothers identified ‘ease and convenience of breastfeeding’ as their overwhelming reason for keeping their infants in bed. Other reasons included the enjoyment of close contact with their baby; anxiety regarding their baby’s health; ease of settling a fractious baby; and a family bed parenting philosophy. In one case, parents slept with their newborn out of necessity rather than choice.
Breastfeeding, bed-sharing and infant sleep
New mothers are often unprepared for either the frequency with which their breastfed newborns need to feed, or how long night-time breastfeeding is likely to continue [28][23]; breastfed babies are generally still feeding as frequently throughout the night at three months of age as they were at one month [29][23]. It has been recognised by various authors that frequent night waking is a factor contributing to the introduction of formula milk to babies, thereby undermining breastfeeding [30][31] given the common (but perhaps erroneous [32]) perception that formula use promotes sleep. For those committed to breastfeeding, sleeping with their babies becomes one of the means by which mothers cope with frequent night-time feeding and later settling [33][22][26].
It was previously observed that mothers who started bed-sharing in their babies’ first month of life were twice as likely to still be breastfeeding when their baby was 4 months of age, in comparison with women who breastfed their baby in the absence of early bed-sharing [23]. It was unclear, however, whether mothers with a commitment to long-term breastfeeding were predisposed to bed-sharing at the outset – or whether there was a physiological connection that linked bedsharing with breastfeeding success. Previous research indicated that when babies bed-share they suckle more frequently at night than when sleeping in their own space [34]. As frequent suckling is well-established as a key factor associated with the successful establishment of breastfeeding, close-contact sleeping arrangements have the potential to enhance breastfeeding rates. Yet standard postnatal ward care (rooming-in) means that babies sleep separately from their mothers in cots.
In order to examine how mother-infant sleep contact might contribute to the establishment and continuation of breastfeeding, Ball et al [35] conducted a randomised controlled trial (RCT) in a UK hospital. Complete details of the trial protocol can be found in the clinical report [35]. Overnight videos were made of mother-baby dyads randomised to 3 sleep locations for their postnatal ward stay: (1) baby in the standard cot at mother’s bedside; (2) baby in a side-car crib attached to mother’s bed; (3) baby in mother’s bed with rail attached to bedside— known as the cot, crib, and bed conditions, respectively. This trial found that babies in the bed or crib exhibited significantly more frequent attempted and successful feeds than those infants in the cot, with no significant differences found in feeding frequency measures between the bed and crib conditions [35]. The use of the stand-alone cot impeded breastfeeding by introducing a barrier between mother and baby preventing contact; inhibited the baby’s ability to root and initiate suckling; obscured the baby’s cues from the mother; and by its height prevented mothers from retrieving their babies without either assistance or the need to get out of bed, thereby substantially hampering the ease and speed of maternal response.
Prompt response to babies’ feeding signals and frequent suckling in the early neonatal period are essential elements in ensuring successful milk production—a process controlled by the hormone prolactin [36][37]. The mother produces more prolactin each time her baby attempts to feed, so frequent attempts are key. Facilitating close maternal–baby proximity during the nights following birth is especially important since breastfeeding at night triggers greater prolactin release than daytime feeding [38][39]. Initial copious milk production (lactogenesis II) is modulated by the amount of prolactin secreted, and frequent stimulation of prolactin secretion in the period between birth and lactogenesis II increases subsequent milk production [40]; infrequent suckling is associated with delayed lactogenesis II [41][42]. The link between frequent early suckling and the timing and volume of copious milk production via prolactin explains the physiological mechanism linking mother-infant sleep contact with improved breastfeeding initiation [43].
In addition to being critical for breastfeeding initiation, high initial prolactin levels are also important for successful long-term lactation. The maintenance of lactation is dependent upon the adequate development of prolactin receptors in breast tissue [44] resulting from frequent feeding in the early days after birth [45]. Prolactin receptors are crucial in maintaining lactation following the switch from endocrine to autocrine control [46]. This means that frequent early feeding will not only lead to effective establishment of milk production, but will enhance its continued maintenance. A common reason given by women for stopping breastfeeding is a perceived or real insufficiency in breastmilk production [25], suggesting inadequate prolactin receptor development in the initial phases of breastfeeding. As this may be a consequence of infrequent feeding bouts, particularly at night, we hypothesised that those infants sleeping in close proximity to their mothers on the postnatal ward in the trial described above (bed or crib) would have better long-term breastfeeding outcomes than infants randomly allocated to the stand-alone cot. To test this hypothesis, telephone interviews at 2, 4, 8, and 16 postnatal weeks ascertained breastfeeding status following hospital discharge. Although all mothers initiated breastfeeding on the postnatal ward, at 16 weeks 43% of babies who were in a separate cot on the postnatal ward were still breastfeeding compared with 73% of the crib group and 79% of the bed group [43]. Although this study was not powered to assess the impact of mother–infant sleep proximity on long-term breastfeeding outcomes, these indicative data suggested that such a trial was warranted; this trial is now underway and due to report in 2010. The evidence to date, however, reinforces the importance of mother-infant sleep contact in facilitating and supporting breastfeeding. Whether or not side-car cribs would be beneficial in the home environment or in the presence of certain bed-sharing contraindications (e.g. premature infants or extremely tired parents etc.) awaits the results of future research.
Some authorities suggest parent-baby bedsharing is a questionable practice that should be abandoned by parents and discouraged by health professionals due to concerns regarding risk of SIDS and/or accidental death [47][48][49]. Such recommendations acknowledge little or no value in mother–infant sleep contact. This view is primarily based on epidemiological studies that calculate the likelihood of SIDS or accidental infant deaths, based on the characteristics of babies who died compared with matched controls in large population-based studies. Babies sleeping on their front, parental smoking, poverty, and young maternal age are all well-known factors that are associated with an increased risk of unexpected infant death [50]. However, estimates of the relative risk of SIDS in the context of bed-sharing vary widely. Although McKenna [51] hypothesised a protective effect of bedsharing on SIDS-risk based on an evolutionary perspective, epidemiological studies have only found a protective effect for room-sharing (co-sleeping). Assessments of the impact of bed-sharing on SIDS-risk in the UK range from no increased risk to babies of non-smoking parents to a 12-fold increase for infants sharing a sofa for sleep with a parent who smokes [52]. The picture is obscured because studies from different countries use different criteria to define bedsharing [53][54][55][56] and have produced a confusing array of statistics that cannot easily be compared [57][58]. Hauck et al [53], for instance, included parents and other carers in the same bedsharing category in her study of bedsharing in Chicago, while the ECAS (European Concerted Action on SIDS) study [54] defined bedsharing as sleeping with one or both parents. A Scottish case-control study of SIDS[55] included in the cases of ‘bedsharing deaths’ not only those infants found dead in an adult bed, but also infants who died in a cot but who had been in their parents bed previously the same night, while a recent Irish case-control study [56] included sofasharing deaths in the bedsharing definition. These varying definitions means that in attempting to ascertain what are the truly risky elements of bedsharing that parents should be warned of we must dig deeply into the ways the various studies were conducted and not simply rely upon the authors’ (or media’s) headline conclusions. Furthermore, these studies consistently ignore infant feeding data in calculating relative risks associated with bed-sharing. Until more appropriate data are collected it is impossible to ascertain whether breastfeeding–related sleep contact between mothers and babies constitutes a risk to babies. However, it is unlikely that any potential risk would be of great magnitude [59] given that breastfeeding is associated with a reduced SIDS risk compared to formula-feeding in several studies [53][60][61].
The key issues underpinning conflicting views of bed-sharing revolve around WHO is bed-sharing; the circumstances under which bed-sharing is taking place (WHERE and HOW), and the way in which bedsharing is conducted (WHAT).
Numerous publications on mother-baby sleep behaviour have documented how mother–baby dyads who routinely bedshare and breastfeed sleep in close proximity with a high degree of mutual orientation (facing one another) and arousal overlap (waking at the same time) (see [62] for comprehensive review). In recent years these studies have been replicated in at least three different settings, and breastfeeding dyads have been observed displaying consistent bed-sharing behaviour, regardless of whether they slept in a narrow hospital bed, a full-size bed in a sleep lab, or at home in beds ranging from twin to king-sized [63][64][65]. Mothers sleep in a lateral position, facing their baby, and curled up around them. Babies, positioned level with their mother’s breasts, sleep in the space created between the mother’s arm (positioned above her baby’s head) and her knees (drawn up under her baby’s feet) [63][64][65]. The cumulative results of these studies provide a robust understanding of breastfeeding–related bed-sharing behaviour and suggest that mothers’ characteristic sleep position represents an instinctive behaviour on the part of a breastfeeding mother to protect her baby during sleep [67]. Although this behaviour evolved in a very different sleep context than involving Western beds and bedding, the principle of infant protection is no less effective. When breastfeeding mothers sleep with their babies they construct a space in which the baby can sleep constrained by their own body, protected from potentially dangerous environmental factors—be they predators, cold weather, the suffocation hazards of quilts and pillows, or the overlaying risk of bed-partners.
Bed-sharing babies of breastfeeding mothers appear, then, to avoid the presumed hazards of sleeping in adult beds (e.g., suffocation, overlaying, wedging, entrapment) [68], due to the presence and behaviour of their mothers. Interestingly, however, differences have been observed in bed-sharing behaviour between breastfeeding and formulafeeding mothers and babies [64]. In a study comparing families videoed sleeping in their home environment, formula-fed infants were generally placed high in the bed, with babies at parental face-height, and positioned between, or on top of, parental pillows. In contrast, breastfed babies were always positioned flat on the mattress, below pillow height and level with the mother’s chest. Formula-feeding mothers spent significantly less time facing their baby and in mutual face-to-face orientation than did breastfeeding mother–baby pairs, and they did not adopt the ‘protective’ sleep position with the same degree of consistency. Breastfeeding mothers and babies experienced a significantly greater frequency of arousals from sleep, and significantly more of these were synchronous (mother and baby waking together) than among formulafeeding mothers and babies [64].
The patterning of these differences is consistent with an understanding of the physiological mechanisms mediating maternal and infant behaviour, in that breastfeeding mothers experience a hormonal feedback cycle, which promotes close contact with, heightened responsiveness towards, and bonding with infants in a way that is absent or greatly diminished among mothers who do not breastfeed [69]. The implication here—that breastfeeding mothers and babies sleep together in qualitatively and significantly quantitatively different ways than do nonbreastfeeding mothers and babies—suggest that epidemiological studies of bed-sharing that have not considered feeding type as a variable for matching cases and controls may have drawn inappropriate results in assessing risk factors associated with bed-sharing. Hopefully epidemiologists will re-examine these issues.
The implications of these studies for bed-sharing by parents who feed their infants formula remain ambiguous. Although we have some evidence that mothers who previously breastfed, or who commenced breastfeeding and then switched to formula, retain the bed-sharing characteristics of breastfeeders [69] it is currently unknown whether parents who have never breastfed can learn to sleep with their infants in the same manner. While it would make common sense to ensure that mothers who have never breastfed, and fathers who sleep alone with their babies, are aware of what safe bedsharing positioning and behaviour entail we do not currently know whether they are likely to maintain the same level of vigilance and synchrony during sleep that is exhibited by breastfeeding mothers. For the time being some authorities suggest that non-breastfeeders keep their baby in a cot by the bed for sleep [70].
In the meantime parents need information with which to make informed decisions, and should be encouraged to weigh up any potential risks and benefits of bed-sharing in light of their own individual circumstances. All parents should be provided with information regarding a) factors known to increase the risk of SIDS in the bed-sharing environment, including parental smoking (particularly maternal smoking in pregnancy), young maternal age, infant prematurity; and b) aspects of adult beds that should be modified with infant safety in mind: e.g. gaps between bed and wall or other furniture, proximity of baby to pillows, type of bedding used, parental behaviour prior to bed-sharing such as consumption of alcohol, drugs or medication affecting arousal. Such information is clearly detailed in the UNICEF leaflet ‘Sharing a Bed with your baby’ [70] and on the NCT website [71].
There is no easy ‘one size fits all’ advice available for the complex issues surrounding a topic such as bed-sharing: it is unrealistic to expect that there ever will be.
Implications for maternity services
Over the past several years, fluctuating advice regarding the relative risks associated with bed-sharing, and a certain amount of media scaremongering, has prompted NHS trusts to remove bedsharing information from patient areas and introduce restrictive policies on what health professionals can say to parents about where their new baby might sleep. This position undermines parents’ rights to make an informed choice on this issue. Maternity services should be aiming to provide parents with balanced information on both the potential pros and cons of bedsharing, including recent research on both lactation and SIDS. The position of the Royal College of Midwives on the obligation of midwives to provide clear information on all aspects of bedsharing is unambiguous [72].
This article was reprinted with permission from the author, Dr. Helen Ball.
This article was reprinted with permission from NCT the UKs largest parenting charity visit www.nct.org.uk for more information. NCT also makes available alongside sleepers go to http://www.nctshop.co.uk/ to see the full range.
——————————————————————————————————————————————
References
1. Pond CM. The significance of lactation in the evolution of mammals. Evolution 1977;31(1):177-99.
2. Small MF. Our babies, ourselves: how biology and culture shape the way we parent. New York: Anchor Books; 1999.
3. Hrdy SB. Mother nature: a history of mothers, infants and natural selection. New York: Ballantine; 1999.
4. Jelliffe DB, Jelliffe EF. Human milk in the modern world: psychosocial, nutritional and economic significance. Oxford: Oxford University Press; 1978.
5. Ball HL. Night-time infant care: cultural practice, evolution, and infant development. In: Liamputtong P, editor. Childrearing and infant care issues: a cross-cultural perspective. Melbourne, Australia: Nova Science; 2006.
6. Crawford M. Parenting practices in the Basque country: implications of infant and childhood sleeping location for personality development. Ethos 1994;22(1):42-82.
7. Valentin SR. Commentary: sleep in German infants—the “cult” of independence. Pediatrics 2005;115(1Suppl):269-71.
8. Javo C, Ronning JA, Heyerdahl S. Child-rearing in an indigenous Sami population in Norway: a cross-cultural comparison of parental attitudes and expectations. Scand.J Psychol 2004;45(1):67-78.
9. Morelli GA, Rogoff B, Oppenheim D, et al. Cultural variation in infants’ sleeping arrangements: questions of independence. Developmental Psychology 1992;28(4):604-13.
10. Jenni OG, O’Connor BB. Children’s sleep: an interplay between culture and biology. Pediatrics 2005;115(1 Suppl):204-16.
11. Hardyment C. Dream babies: child care from Locke to Spock. London: Jonathan Cape; 1983.
12. Blum D. Love at Goon Park: Harry Harlow and the science of affection. Cambridge, Mass.: Perseus Books; 2002.
13. Korner AF, Thoman EB. The relative efficacy of contact and vestibular-proprioceptive stimulation in soothing neonates. Child Dev 1972;43(2):443-53.
14. Christensson K, Siles C, Moreno L, et al. Temperature, metabolic adaptation and crying in healthy full-term newborns cared for skin-to-skin or in a cot. Acta Paediatr 1992;81(6-7):488-93.
15. Ludington-Hoe SM, Johnson MW, Morgan K, et al. Neurophysiologic assessment of neonatal sleep organization: preliminary results of a randomized, controlled trial of skin contact with preterm infants. Pediatrics2006;117(5):e909-e923.
16. Ferber SG, Makhoul IR. The effect of skin-to-skin contact (kangaroo care) shortly after birth on the neurobehavioral responses of the term newborn: a randomized, controlled trial. Pediatrics 2004;113(4):858-65.
17. Anderson GC, Moore E, Hepworth J, et al. Early skin-to-skin contact for mothers and their healthy newborn infants. Birth 2003;30(33):206-7.
18. O’Connor S, Vietze PM, Sherrod KB, et al. Reduced incidence of parenting inadequacy following rooming-in. Pediatrics 1980;66(2):176-82.
19. Barr RG, Trent RB, Cross J. Age-related incidence curve of hospitalized Shaken Baby Syndrome cases: convergent evidence for crying as a trigger to shaking. Child Abuse and Neglect 2006;30(1):7-16.
20. Gerhardt S. Why love matters: how affection shapes a baby’s brain. Hove, East Sussex: Brunner-Routledge; 2004.
21. Davies DP. Ethnicity and SIDS: what have we learnt? Early Hum Dev 1994;38(3):215-20.
22. Ball HL. Reasons to bed-share: why parents sleep with their infants. Journal of Reproductive and Infant Psychology 2002;20(4):207-21.
23. Ball HL. Breastfeeding, bed-sharing, and infant sleep. Birth 2003;30(3):181-8.
24. Blair PS, Ball HL. The prevalence and characteristics associated with parent-infant bed-sharing in England. Arch.Dis.Child 2004;89:1106-10.
25. Bolling K, Grant C, Hamlyn B et al. Infant Feeding Survey 2005. London: The Information Centre for Health and Social Care; 2007. Available from: ttp://www.ic.nhs.uk/statistics-and-datacollections/health-and-lifestyles-related-surveys/infantfeeding-survey
26. McCoy RC, Hunt CE, Lesko SM, et al. Frequency of bed sharing and its relationship to breastfeeding. J Dev Behav.Pediatr 2004;25(3):141-9.
27. Ball HL, Hooker E, Kelly PJ. Where will the baby sleep? Attitudes and practices of new and experienced parents regarding cosleeping with their newborn infants. American Anthropologist 1999;101(1):143-51.
28. Greenslade J. What’s best about breastfeeding? NurseryWorld 1995;(January):19-21.
29. Elias MF, Nicolson NA, Bora C, et al. Sleep/wake patterns of breast-fed infants in the first 2 years of life. Pediatrics 1986;77(3):322-9.
30. Pinilla T, Birch LL. Help me make it through the night: behavioral entrainment of breast-fed infants’ sleep patterns. Pediatrics 1993;91(2):436-44.
31. Marchand L, Morrow MH. Infant feeding practices: understanding the decision-making process. Fam Med 1994;26(5):319-24.
32. Doan T, Gardiner A, Gay CL, et al. Breast-feeding increases sleep duration of new parents. J Perinat.Neonatal Nurs 2007;21(3):200-6.
33. Morgan KH, Groer MW, Smith LJ. The controversy about what constitutes safe and nurturant infant sleep environments. J Obstet Gynecol Neonatal Nurs 2006;35(6):684-91.
34. McKenna JJ, Mosko SS, Richard CA. Bed sharing promotes breastfeeding. Pediatrics 1997;100(2 Pt 1):214-9.
35. Ball HL, Ward Platt MP, Heslop E, et al. Randomised trial of infant sleep location on the postnatal ward. Arch Dis Child 2006;91(12):1005-10.
36. Johnston JM, Amico JA. A prospective longitudinal study of the release of oxytocin and prolactin in response to infant suckling in long term lactation. J Clin Endocrinol.Metab 1986;62(4):653-7.
37. Uvnas-Moberg K, Widstrom AM, Werner S, et al. Oxytocin and prolactin levels in breast-feeding women. Correlation with milk yield and duration of breast-feeding. Acta Obstet Gynecol Scand. 1990;69(4):301-6.
38. Tennekoon KH, Arulambalam PD, Karunanayake EH, et al. Prolactin response to suckling in a group of fully breast feeding women during the early postpartum period. Asia Oceania J Obstet Gynaecol 1994;20(3):311-9.
39. Woolridge MW. Baby-controlled breastfeeding. In: Stuart-Macadam P, Dettwyler KA, editors. Breastfeeding: biocultural perspectives. New York, NY: Aldine de Gruyter; 1995. pp. 217-42
40. Neville MC, Morton J, Umemura S. Lactogenesis. The transition from pregnancy to lactation. Pediatr Clin North Am 2001;48(1):35-52.
41. Chapman DJ, Perez-Escamilla R. Identification of risk factors for delayed onset of lactation. J Am Diet.Assoc. 1999;99(4):450-4.
42. Sozmen M. Effects of early suckling of cesarean-born babies on lactation. Biol Neonate 1992;62(1):67-8.
43. Ball HL. Evolutionary paediatrics: a case study in applying Darwinian medicine. In: Elton S, O’Higgins P, editors. Medicine and evolution: current applications, future prospects. New York: Taylor & Francis; 2008. pp. 127-52
44. Riordan J. Breastfeeding and human lactation. 3rd edition Sudbury, Massachusetts: Jones and Bartlett; 2005.
45. Marasco L, Barger J. Cue feeding: wisdom and science. Breastfeeding Abstracts 1999;18(4):28-9.
46. Lawrence RA. Breastfeeding: a guide for the medical profession. 5th revised edition St Louis: Mosby; 1999.
47. Ateah CA, Hamelin KJ. Maternal bedsharing practices, experiences, and awareness of risks. Journal of Obstetric, Gynecologic, and Neonatal Nursing 2008;37(3):274-81.
48. Byard RW. Is co-sleeping in infancy a desirable or dangerous practice? J Paediatr Child Health 1994;30(3):198-9.
49. Weale S. Too close for comfort? [Accessed 15 September 2009]. Available from: http://www.guardian.co.uk/society/2003/jan/20/medicineandhealth.publichealth2
50. Fleming PJ. Understanding and preventing sudden infant death syndrome. Curr.Opin.Pediatr 1994;6(2):158-62.
51. McKenna JJ. An anthropological perspective on the sudden infant death syndrome (SIDS): the role of parental breathing cues and speech breathing adaptations. Medical
Anthropology 1986;10(1):9-53.
52. Blair PS, Fleming PJ, Smith IJ, et al. Babies sleeping with parents: case-control study of factors influencing the risk of the sudden infant death syndrome. CESDI SUDI research group. BMJ 1999;319(7223):1457-61.
53. Hauck FR, Herman SM, Donovan M, et al. Sleep environment and the risk of sudden infant death syndrome in an urban population: the Chicago Infant Mortality Study.
Pediatrics 2003;111(5 Part 2):1207-14.
54. Carpenter RG, Irgens LM, Blair PS, et al. Sudden unexplained infant death in 20 regions in Europe: case control study. The Lancet 2004;363:185-91.
55. Tappin D, Ecob R, Brooke H. Bedsharing, roomsharing and sudden infant death syndrome in Scotland: a case-control study. Journal of Pediatrics 2005;147(1):32-7.
56. McGarvey C, McDonnell A, Hamilton K, et al. Bed sharing and sudden infant death syndrome: Irish case-control study. Paediatr Child Health 2006;11(Supp A):19A-21A.
57. Cote A. Bed sharing and sudden infant death syndrome: do we have a definition problem? Paediatr Child Health 2006;11(Suppl A):34A-8A.
58. Horsley T, Clifford T, Barrowman N, et al. Benefits and harms associated with the practice of bed sharing: a systematic review. Arch Pediatr Adolesc Med 2007;161(3):237-45.
59. Leduc D, Camfield C. Putting sudden infant death syndrome research into practice: paediatricians’ perspective. Paediatr Child Health 2006;11(Suppl A):51A-2A.
60. Hoffman HJ, Damus K, Hillman L, et al. Risk factors for SIDS. Results of the National Institute of Child Health and Human Development SIDS Cooperative Epidemiological Study. Ann.N Y.Acad Sci. 1988;533:13-30.
61. Vennemann MM, Bajanowski T, Brinkmann B, et al. Does breastfeeding reduce the risk of sudden infant death syndrome? Pediatrics 2009;123(3):e406-e410.
62. McKenna JJ, Ball HL, Gettler LT. Mother-infant cosleeping, breastfeeding and sudden infant death syndrome: what biological anthropology has discovered about normal infant sleep and pediatric sleep medicine. Am J Phys.Anthropol. 2007;Suppl 45:133-61.
63. Baddock SA, Galland BC, Bolton DP, et al. Differences in infant and parent behaviors during routine bed sharing compared with cot sleeping in the home setting. Pediatrics 2006;117(5):1599-607.
64. Ball H. Parent-infant bed-sharing behavior: effects of feeding type and presence of father. Human Nature 2006;17(3):301-18.
65. Young J, Fleming PJ, Blair P et al. Night-time infant care practices : a longitudinal study of the importance of close contact between mothers and their babies. Deutscher Stillund Laktationskongress May 2001. Stillmanagement und Laktation. Leipzig, Germany: Leipziger Universitätsverlag; 2002.
66. Richard C, Mosko S, McKenna J, et al. Sleeping position, orientation, and proximity in bedsharing infants and mothers. Sleep 1996;19(9):685-90.
67. Ball HL. Breastfeeding and mother-infant sleep proximity: implications for infant care. In: Trevathan W, Smith EO, McKenna J, editors. Evolutionary medicine and health: new perspectives. New York: Oxford University Press; 2007. pp.226-41
68. Nakamura S, Wind M, Danello MA. Review of hazards associated with children placed in adult beds. Arch Pediatr Adolesc Med 1999;153(10):1019-23.
69. Uvnas-Moberg K. The oxytocin factor: tapping the hormone of calm, love and healing. Cambridge, MA.: Da Capo Press; 2003.
70. UNICEF UK Baby Friendly Initiative. Sharing a bed with your baby: a guide for breastfeeding mothers. Available from: http://www.babyfriendly.org.uk/pdfs/sharingbedleaflet.pdf
71. NCT Position statement: co-sleeping and bed-sharing. Available from:
72. Royal College of Midwives. Bed-sharing and cosleeping: Position Statement No. 8.







So nice to read a well researched co-sleeping article, especially one that properly explores the relationship between breastfeeding and co-sleeping. Fab!
[…] Evolutionary Parenting has a detailed article on from Helen Ball, an authority on the issues associated with co-sleeping. […]
I posted this wonderful article in my weekly links post today: http://freeyourparenting.com/2011/11/20/sharing-sunday-17/
Wonderful! I believe the more people that can read Dr. Ball’s work, the better!!!
Great article – as a breastfeeding mother and cosleeper myself its nice to see a well balanced discussion of the facts and history behind it.
[…] Bed-Sharing and Co-Sleeping: Research Overview Dr. Sears Addresses Recent Co-Sleeping Concerns Co-Sleeping Safety […]
[…] enjoyable, and as something that could actually benefit my child. There are psychological and biological reasons why bed-sharing is A Very Good […]
[…] has shown that in early months, co-sleeping helps to support breastfeeding and lowers SIDS risk. It also helps moms get more sleep and helps baby feel more secure (and thus, […]
[…] Bed-Sharing and Co-Sleeping: Research Overview Dr. Sears Addresses Recent Co-Sleeping Concerns Co-Sleeping Safety Share this:TwitterFacebookLike this:LikeBe the first to like this post. This entry was posted in Attachment Parenting and tagged attachment parenting, bed time, bed-sharing, breastfeeding, challenging, co-sleeping, sleep. Bookmark the permalink. Special Time → […]
Could I print this article to give out at my parenting group?
Please do!
May I put a link to this excellent article and quote from it on my website?
Sure 🙂
[…] sleep, so cosleeping it was. I believe there are many benefits to sleeping with your baby, and new research is showing that the risks that the general public is concerned about are significantly lessened […]
[…] You have told me your opinion and your husband’s opinion regarding where baby should sleep. There is one more opinion that deserves consideration, and that is the opinion of the one who is sleeping – the baby! Nestled in the arms of a parent, comforted by human warmth, sound and breathing rhythms, babies sleep and learn about the world around them. Unlike other primates that "cling" to their mothers, "human infants are dependent upon their mothers to ensure that proximity is maintained," says Professor Helen Ball of the Parent-Infant Sleep Lab of Durham University in her article Bed Sharing and Co-Sleeping: Research Overview . […]
[…] McKenna and Dr. Helen Ball of the Parent-Infant Sleep Lab at Durham University, when done safely, mother-infant bedsharing can improve nighttime breastfeeding, extend the duration of breastfeeding, contribute to infant and maternal health and wellbeing, and […]
[…] [11] https://gku.flm.mybluehost.me/evolutionaryparenting.com/bed-sharing-and-co-sleeping-research-overview/ […]
Tracey have you read or heard any information on the prospect that SIDS, true SIDS with no suffocation in blankets etc may actually be related to the infants heart suddenly stopping unexplainably I think smoking etc may affect this however it could be predisposed and genetic and maybe all our SIDS prevention is futile and it has only prevented suffocation etc?!
I mentioned the genetic predisposition in another piece (trying to remember which one). However, being a predisposition does not mean it won’t pass, so much of the research is probably still valid. For example, formula is linked to higher SIDS risk, but why? We don’t know for certain, and it may only interact for a child with this predisposition. But it doesn’t mean understanding the link to formula isn’t key – just that removing formula won’t solve it completely. Make sense?
Cecile asks a good question I can’t resist answering 🙂 There is some evidence that certain infants are more vulnerable to the possibility of SIDS than others — but it appears that 3 things have to happen at the same time for these babies to experience SIDS (this is the Triple-risk model, which is the current best explanation).
For SIDS to happen you appear to need a combination of:
a) a vulnerable infant;
b) a critical developmental period;
c) an external stressor.
Critical period is normally 2-4 months (peak age for SIDS — i.e. when most infants succumb to unexplained and unexpected death). External stressor = one of several possible experiences that ‘might’ challenge the infant physiologically in some way (prone sleeping, head covering/overheating, airway covering/rebreathing etc etc). Vulnerable infant = one who has been developmentally compromised during gestation (e.g. premature, LBW, exposure to smoking or drug use in pregnancy) or postnatally (exposure to smoking, not breastfed etc).
It seems as though SIDS occurs when a vulnerable baby encounters an external stressor during a critical developmental period and experiences some catastrophic failure of the normal protective physiological mechanisms that kick in for all other babies when they experience the stressor. We don’t know all the things that might cause a baby to be vulnerable, but some may be genetic. So all we can currently do is highlight which babies might be most vulnerable, when, and avoid those things that we think are stressors. This is how SIDS prevention guidance is generated. Problem is the vast majority of babies aren’t vulnerable — their normal defences to all the stressors etc work fine — and even potentially ‘vulnerable’ babies can usually cope with stressors unless they are experiencing the ‘critical period’ when some sorts of changes are happening that cause their normal defences to fail. But SIDS-reduction strategies treat all babies as equally vulnerable all the time, and therefore all parents are told to avoid all the known or presumed stressors, even though they are not problematic for the vast majority of babies. So wouldn’t say SIDS prevention is futile — I’d say it is a rather blunt tool as it is currently used. It is improving, but we need to understand more about how to tailor effective info to those whose babies are most likely to be vulnerable.
Thank you so very much 🙂
[…] found that roughly half of all parents bedshare for at least part of the night. When done safely, bedsharing can make nighttime breastfeeding easier, extend the duration of breastfeeding, contribute to infant […]
[…] the way…if you’re drunk or high, someone else better be in charge). For buckets of solid research on this subject along with a complete list of risk factors, check out Evolutionary […]
[…] to be perfectly adapted to their mothers’ bodies. Bed-sharing has also been shown to promote successful breastfeeding, which significantly reduces the risk of SIDS. Out of the millions of years of human history, the […]
[…] not for everyone. BUT, you should plan to share your room. Here’s a great overview of the research on co-sleeping and bedsharing. Even the AAP recommends sharing a room with your baby. (Not that I love the AAP, but I’m […]
[…] Babies should not sleep alone. http://www.naturalchild.org/james_mckenna/cosleeping.pdf https://gku.flm.mybluehost.me/evolutionaryparenting.com/bed-sharing-and-co-sleeping-research-overview/ http://www.smartparenting.com.ph/kids/baby/co-sleeping-is-safer-for-babies-than-cribs-experts-say/page/2 http://www.askdrsears.com/topics/sleep-problems/sids-latest-research-how-sleeping-your-baby-safe Shelley […]
[…] evolutionaryparenting.com […]
[…] Bed-Sharing and Co-Sleeping: Research Overview https://gku.flm.mybluehost.me/evolutionaryparenting.com/bed-sharing-and-co-sleeping-research-overview/ […]
[…] http://www.cientistaqueviroumae.com.br/2013/06/cama-compartilhada-protecao-amor-e.html Cama compartilhada: por que é bom e seguro? – Cientista Que Virou Mãe http://www.cientistaqueviroumae.com.br/2012/03/cama-compartilhada-por-que-e-bom-e.html Bedsharing and SIDS: The Whole Truth – Evolutionary Parenting https://gku.flm.mybluehost.me/evolutionaryparenting.com/bedsharing-and-sids-the-whole-truth/ The Do’s and Don’ts of Co-Sleeping – Evolutionary Parenting https://gku.flm.mybluehost.me/evolutionaryparenting.com/the-dos-and-donts-of-co-sleeping/ Bed-Sharing and Co-Sleeping: Research Overview – Evolutionary Parenting https://gku.flm.mybluehost.me/evolutionaryparenting.com/bed-sharing-and-co-sleeping-research-overview/ […]
[…] are many benefits to co-sleeping. According to co-sleeping advocates Dr. Sears, Evolutionary Parenting, WBUR (Boston’s NPR news station), co-sleeping expert Dr. James McKenna, and other sources, some […]
[…] questo studio sottolinea che la condivisione del letto, inoltre, favorisce l’allattamento al seno e contribuisce ad abbassare il livello di cortisolo, un ormone legato alle condizioni di […]
[…] Bed-Sharing and Co-Sleeping: Research Overview […]
Excellent article. I wish I found this sooner. Thank you!
[…] de borst te geven. Op verzoek voeden past niet alleen goed bij natuurlijk ouderschap , maar uit onderzoek blijkt dat moedermelk ervoor is gemaakt om naar believen te worden […]
[…] Bed-Sharing and Co-Sleeping: Research Overview – Evolutionary Parenting: link. […]
[…] Bed-Sharing and Co-Sleeping: Research Overview […]