By Shannon Connors
 I awoke on Tuesday, December 10th, 2013 at 4:45 am, after about five hours of broken sleep. I showered using the Chlorhexidine soap, changed and grabbed my last-minute items. My husband, Luke and I were en route to Sunnybrook Hospital by 5:45 am on a cold, cold morning. Luke dropped me off at the M wing doors of Sunnybrook right on time at 6 am and I checked into obstetrical triage while he parked. What a different feeling it was to arrive at the hospital not in labour! It was great being able to walk right in by myself, feeling ready and excited. I was the only patient to be found at this time in triage and was happily surprised at the calm, ‘chilled-out vibe’ of our lovingly anticipated Birth Day. Luke and I watched TV and surfed our iphones while relaxing in the lounge recliners. I had had to stop eating at midnight and could not drink even water after 4 am.
I awoke on Tuesday, December 10th, 2013 at 4:45 am, after about five hours of broken sleep. I showered using the Chlorhexidine soap, changed and grabbed my last-minute items. My husband, Luke and I were en route to Sunnybrook Hospital by 5:45 am on a cold, cold morning. Luke dropped me off at the M wing doors of Sunnybrook right on time at 6 am and I checked into obstetrical triage while he parked. What a different feeling it was to arrive at the hospital not in labour! It was great being able to walk right in by myself, feeling ready and excited. I was the only patient to be found at this time in triage and was happily surprised at the calm, ‘chilled-out vibe’ of our lovingly anticipated Birth Day. Luke and I watched TV and surfed our iphones while relaxing in the lounge recliners. I had had to stop eating at midnight and could not drink even water after 4 am.
Cruelly, Luke scarfed down a coffee and muffin right in front of me!
At around 7 am, a nurse named Maureen led us to the recovery room to which we would return post-birth. There, I met the anesthetist who would give me my spinal block and monitor me during surgery. Having endured two previous long labours, which both culminated in emergency C-sections, scheduling this one had seemed like the right, logical thing to do. With our first daughter, my labour stalled for many hours at 6 cm dilation. With our second daughter, I didn’t go into labour until 42 weeks, believing that avoiding induction was best for a VBAC. I had researched VBACs, hired a doula with a very high VBAC success rate, switched from OB to midwife mid-pregnancy and done everything I could to create the conditions for a successful VBAC with my second. I had even delayed pain relief for so long that my midwife finally suggested I get the epidural in order to help me relax. Although I was having transition-like contractions which were intensified by back labour, I never dilated past 4 cm. My second daughter was born not breathing for two long minutes having swallowed the meconium. Because of all this, Luke definitely believed an elective cesarean was the safest option for both baby and me – and the only option as far as he was concerned.
About halfway through this pregnancy, it had seemed like all the stars had aligned just for me, when I learned of an opportunity to have a “natural Cesarean section” – the first ‘official’ one to be performed in Canada! My midwife, Nicole Romeiko, set up a meeting with the OB, Dr. Jon Barrett, who excitedly explained to me that the main distinguishing features of a natural Cesarean is early skin-to-skin contact with the mother and that I would be encouraged to push in the hopes that I would be a more active participant in the birth. Dr. Barrett encouraged me to watch the video on youtube which you can find here: http://www.youtube.com/watch?v=m5RIcaK98Yg and I also read an article about it here: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2613254/.
Well, the time had finally arrived. Now, in the moments prior to entering the operating theatre, I became frightened and anxious in the way one would before any elective surgery. I was so grateful to have my midwife Nicole at my side. She encouraged me to cry and talk my fears out to her. She listened, accepted, rationalized and normalized them for me. This cathartic release meant that I did not have to bring these same fears into the OR with me.
Once in the OR, I was seated on the operating table for the spinal. I was given some warm blankets for my lap, which was great because I was freezing cold. Nurse Maureen really comforted me by just sort of holding and hugging me. It helped ease my anxiety about the spinal so much so that when she was called away at one point, I found myself wishing one of the other nurses or residents in the room would’ve taken her place. Of course, it would have been even better if Luke could’ve been in there with me. The process of getting the needle in the right spot was extremely unpleasant.
Finally, the spinal was in. At this point, I experienced a reaction to the spinal that made me feel like I couldn’t breathe. The anesthetist explained that this was because some of my organs were frozen. However, my diaphragm was not, so breathing would not be affected. Nonetheless, I was experiencing what felt like crushing chest pain and as though each breath might be the last I was able to take. I was unable to cough or swallow. I was assured this was all normal and would pass. Once again, Nicole was my saving grace. I told her how I felt and asked her if she could help me breathe. She told me that all I needed to do was to feel my breath going in and out of my nose. Once I focused on breathing through my nose, I was able to stop panicking.
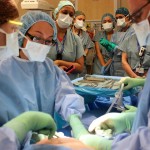
By the time I saw Luke again all the scary stuff had passed. I cried in both relief and release. He was smiling with the camera around his neck looking so excited. This made me feel worlds better than I had just a moment ago. Dr. Barrett smiled confidently at me and Luke, asked how I was doing, and proceeded to give instructions to his team. I learned later that Luke had been pacing madly in the recovery room for the 30 or so minutes we were separated, anxious about something going wrong. I also learned later he felt reassured by Dr. Barrett’s confidence.
Earlier, Dr. Barrett had put my catheter in and before I knew it, I asked and was told that my belly was open! There was lots of pulling and tugging that I could sort of see happening but not really feel. This part seemed to take quite a while and at one point I (mostly) jokingly asked Nicole, “There is a baby in there, right?”
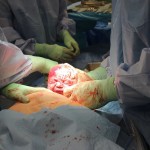
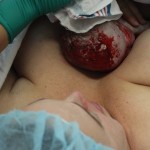
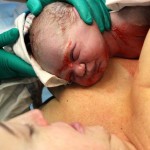
Then came the moment where Dr. Barrett asked me to ‘push’ – to bear down as if I were having a bowel movement. I tried to visualize it but I didn’t actually feel as though I had any control or ability to make any movement whatsoever. Then, the drape was quickly lowered (I had asked for the drape to be lowered when the baby was coming out) and I just caught the wondrous image of my baby’s head being lifted out! I was so relieved to hear little crying noises soon after. Then, my baby was being passed under the drape to Nicole who put him immediately on my chest as his cord pulsed out. Incidentally, the cord had been wrapped around the baby’s neck and, although he wasn’t breech after all, that in itself may have necessitated another emergency C-section had I attempted a third trial of labour.
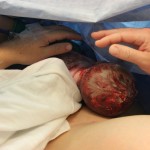
The feeling of having my baby go directly from my belly into my arms where he would stay – for all but a brief moment when Nicole weighed him about a half hour later – is truly indescribable. It was just so incredible yet felt so very natural and so right. It felt dramatically different, the opposite really, of how my past two births had felt. Those times, of course, my baby had been immediately whisked away to the other side of the room for what seemed like forever until I could hold them and longer still till I could put them to the breast in the recovery room.
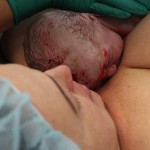
I loved that my newborn son had blood and fluid and vernix all over him when he came to me. He was toweled off a bit and a flannel sheet was placed over him. My son and I were skin-to-skin and would remain so almost exclusively for the next several consecutive days! I believe in and am witness to the undeniable importance of skin-to-skin with the mother for at least those first two crucial hours after birth but also the following few days in order to establish breastfeeding and bonding. Our son, Leif, ‘crawled’ to the breast partly on his own and remained there eagerly for a good part of our first few days (weeks, months…) together.
Looking back now, it hasn’t been perfect. Leif was tongue-tied and I have had issues with my milk supply, as I have with my past pregnancies. However, I am secure in the knowledge that we had the best birth possible and the best possible start to our bonding and breastfeeding relationship. My son’s birth exceeded my expectations and left me feeling satisfied and proud of the whole experience. This is in sharp contrast to the feelings of let down and failure of my previous two unplanned c-sections. Although I definitely experienced some baby blues and even some PPD with those two births, I have felt nothing of the sort with this birth (at two months post-partum).
I’m so thankful to Nicole for bringing this opportunity to my attention and to Dr. Barrett for his interest and expertise in helping me – and hopefully many, many more women for whom a successful vaginal birth is unlikely or impossible – to have this truly beautiful, truly amazing birth experience.






Thank you so much for sharing your story. I wanted to have a natural birth with my daughter and even though I knew there were no guarantees I thought that there was no way I would end up with a C-section. After 36 hours of intense back labor and stopping at 7 cms, I chose to finally get an epidural and let them break my water. We found out that there was meconium in the fluid and after two hours of still no progression my little girl’s heartrate started to drop after each strong contraction. For her safety we decided to have a C-section. I could not do skin to skin immediately after as they needed to suction out her respiratory tract (because of the meconium), but my husband was actually able to go with her and do skin to skin. I loss a lot of blood and was very weak from labor and surgery, however once in the recovery room a nurse brought my daughter to me and helped me nurse her and be skin to skin. I had to stay in recovery for 12 hours after surgery do to fever and the need for a blood transfusion, so I didn’t get to have visitors. My husband did bring my daughter out for my family to see but I had limited contact with family and friends. I have always felt saddened that the birth did not go as I wanted and in a way felt like less of a woman for having a C-section. I know that it is not true, but I keep thinking what more could I have done to make sure I had a natural vaginal birth. Your story really helps me see that it’s ok to have a C-section, even a planned one. With mine not being planned I was so exhausted and drained from labor, I didn’t get to feel that real connection and happiness directly after birth. I love my daughter and I’m so happy that she was born healthy and beautiful. I still debate with my next child if I want to try a VBAC or just do a scheduled C-section to avoid the exhaustion and distance that I had with my first.
Thank you again. Your story has given me new insite to my situation.
I’m so happy to read this! I know if I have another baby it will be by scheduled c-section because I had PROM at 34 weeks with my first, and he was breech, so the incision had to be vertical, negating the possibility of a VBAC. I was shown my baby for about 2 seconds and then he was taken to the NICU and I didn’t get to see him for another 6-7 hours (and even then I was only allowed to hold him for an hour or two a day for the first week). I had wanted a natural water birth, and knowing I will never be able to even attempt natural labor is really hard for me. Your experience gives me some hope that I can at least get the skin-to-skin immediately and keep my baby with me! Thanks for sharing!
[…] Shannon Connors natural c-section story on Evolutionary Parenting (USA) […]
[…] Birth Story: My Natural Cesarean Section evolutionaryparen… […]