A new article in Pediatrics “Room-sharing at ages 4 and 9 months is associated with less nighttime sleep in both the short and long-term, reduced sleep consolidation, and unsafe sleep practices previously associated with sleep-related death.” Those are some pretty strong suggestions for a study and as the authors call for the AAP to revisit their entire stance on room-sharing, it begs the question of what type of research they have to back this up and whether or not it is warranted. Furthermore, outside of this one study, it is worth examining the idea of babies sleeping alone and what we know about this practice as it is so biologically and evolutionarily abnormal. But let’s start with the study at hand. What is the INSIGHT Study? The current examination groups the control and intervention group, but of course there are bound to be differences between them. The control group may not have weaned a child off feeds or have been conditioned to ignore their child at night. These are important elements that need to be considered when we look at the data as a whole. We also need to be aware that this study is really all about moving infants away from what is biologically normal. *** Does Room-Sharing Lead to Worse Sleep? One of the main findings that is getting lots of traction in the media is the idea that babies who sleep independently early get “better” sleep as measured by more sleep and greater consolidation. Of note, herein independent sleep is simply sleeping in one’s own room and not room-sharing per the AAP’s guidelines. According to this study – which included 230 mother-infant dyads – infants who were sleeping independently at 4 months were getting 40 min more sleep (on average) at 9 months and those who were sleeping independently at 9 months were getting 45 min more sleep at 30 months. At 4 months, independent sleepers had longer stretches of sleep (but not total duration of sleep) and fewer feeds at night (this makes sense given the intervention material stated above). This may sound all fine and dandy, except these findings actually have two MAJOR errors that basically invalidate their conclusions. So what are these major problems? Source: North Country Neurology Most importantly, infant sleep is parent reported. Although this had been a staple of understanding infant sleep for years, research that has examined parent report relative to actigraphy[2][3][4][5] has found that the two diverge quite readily. Importantly, infants are waking and up much more than parents believe them to be and this is going to be much more likely to be the case when infants are separated from their parents. A baby who rouses briefly in their own room is unlikely to get the attention of a parent, but one who does while sleeping next to mom is more likely to be noticed. To highlight how discrepant this difference can be, we can look at one of the larger studies that included actigraphy to assess infant sleep[2]. In this study, parent diary reports included the number of night wakings they were aware of as well as actigraphy measures of wakings. At baseline, families reported an average of 3.1 wakings per night; however, actigraphy found that infants were waking up on average over 8 times per night. This intervention study also found that although parents who were in the intervention group – which was aimed at teaching independent sleep via controlled crying – reported much improvement in their baby’s sleep relative to the control group, actigraphy again found that there was no difference in sleep quality for babies. They were not sleeping longer or waking less, even though parents reported they were. Interestingly, the researchers do not completely ignore this, stating that they are aware research has found no differences in sleep depending on where a child sleeps[4][5]. However, they argue that this only reinforces how bad cosleeping can be for mothers. As they state, “However, this possibility, if true, would only reinforce the concept that room-sharing may result in either unnecessary parental responses to infant night wakings or, alternatively, the infant’s expectation of caretaking behaviors from parents, both of which can be expected to lead to decreased sleep for infant and parent.” (p 7) Now, as we know, it doesn’t lead to worse sleep for infants and as for mothers, although some would suggest maternal sleep is worse (e.g., [4]), this contradicts research that has found breastfeeding, cosleeping dyads sleep better than their solitary sleeping counterparts[6][7]. The second error is that this study fails to consider the third variable problem. That is, it is entirely likely that there is a child characteristic that has an influence on where they sleep and how well they sleep. A child with a feeding problem will wake more to feed more and is more likely to be kept close to facilitate these feedings. Similarly, a child that sleeps through early is more likely to be moved to his or her own room early. This is important as we look to the 30-month findings that saw lower nighttime sleep in those who were still room-sharing at 9 months versus those who were not. It seems strange to consider that room-sharing 21 months earlier would have such a profound effect; however, it is not strange to consider that these children could be different in other ways. For example, more of them may still be room-sharing and thus we simply have more accurate data on sleep duration. These children may be home during the day and thus napping more (after all, there was no difference in total daily sleep so these children were just napping longer during the day). Another element that speaks to this problem is breastfeeding rates. The group that was sleeping alone by 4 months had lower rates of breastfeeding (≥ 80% of the time) than those who were sleeping alone by 9 months; however, the group with the lowest rates of breastfeeding was the group who were still room-sharing at 9 months. Typically breastfeeding and cosleeping go hand-in-hand and so there is the possibility that there were other issues influencing sleep that simply weren’t assessed and controlled for. There are many possibilities that don’t speak to solitary sleep as the cause. Of course, this requires us to accept their sleep data, which we shouldn’t, but provides evidence that even looking at bad data in the best of lights, there is still a major flaw in their conclusions. To answer the question of whether or not room-sharing leads to worse sleep, the data here does not tell us anything from the perspective of infant sleep. In fact, arguably the most accurate responses are from those who are room-sharing as these are the families who are most likely to be aware of the movements and wakings of their child. We certainly don’t have any evidence that there is a causal relationship between solitary sleep and sleep duration. *** Is Room-Sharing Actually Dangerous, as the Researchers Contest? Photo Credit: NPR The secondary conclusion reached by these researchers is that room-sharing is actually dangerous because it increases the risk of bedsharing, something the AAP has spoken out against. The researchers contend that the AAP’s position on room-sharing is not evidence-based as the majority of SIDS deaths occur prior to 6 months and the research the AAP cited does not include cases from 6-12 months. Furthermore, they suggest that the hypothesized protective mechanism in room-sharing may actually be due to bedsharing: Although the Task Force’s recent letter cited more frequent arousals among room-sharers as the potential protective mechanism, the 2 studies referenced do not support that conclusion. The first is a case-control study of 18 infants. Among 9 roomsharers, 5 were bed-sharers, making conclusions about arousals among those who are room-sharing but not bed-sharing (versus independent sleepers) problematic. The second study, which also included bedsharers in the room-sharing group, states that parental presence in the room at bedtime (eg, holding, rocking, feeding to sleep) explained much of the variance in night wakings and that night-long roomsharing had a “negligible (<1%) independent contribution to the explained variance.” These researchers then go on to say that the biggest problem with the room-sharing recommendation is that higher likelihood of bedsharing at 4 and 9 months and therefore a greater risk of SIDS. Because of this, the AAP should revisit their recommendations to room-share for the first year of life when a transition is harder on babies because of separation anxiety. So is room-sharing actually dangerous? Should the AAP revise their stance? No and perhaps. No, room-sharing is not dangerous, but the AAP may want to look more into this link with bedsharing and a protective mechanism. Perhaps we can convince the AAP to suggest safe bedsharing for a spell? *** Is There Cause to Worry About Solitary Sleep for Infants? Not too surprisingly, the researchers seem to ignore some very important elements in their rush to claim cosleeping can have negative consequences for families and the AAP ought to revisit its recommendation to push early solitary sleep. Most importantly I want to reiterate that this entire intervention is based on moving families away from what is biologically normal. It was a pity to see not a single reference to either Dr. McKenna or Dr. Ball, both of whom have looked at the evolution and biology of maternal-infant sleep in depth and whose work should not be ignored here. I strongly recommend anyone interested look up their work (much of which is cited in my various articles on sleep) and see what we know about mother-infant sleep from a much more complete perspective than we see in this study. One of the other elements that is conveniently ignored in this piece (and others on the INSIGHT study) is that there may be evidence that solitary sleep increases the risk of insecure attachment[13]. Now, to be fair here, the research on attachment and sleep location is very preliminary and requires more follow-up to be able to make any conclusion. However, the current study is also quite flawed and any recommendation should not be made on the basis of this study alone. If one wants to take anything from this, one should also take into consideration other studies that also require far more detail and follow-up or replication before making any conclusions. The final issue that was ignored entirely by the researchers is breastfeeding. We can see a bias against breastfeeding when we look at the intervention being promoted. In no way is it biologically appropriate to cut all night feeds by 4 months of age and expect no effects on supply. Further, if the feeding of an infant under 6 months is shared, then it is likely that supplementation is being used (though of course expressed breastmilk could be used too). Clearly the intervention is not geared towards the realities of breastfeeding mothers, but that is simply not part of any discussion herein. The ignorance of how breastfeeding and cosleeping work together is hugely problematic and I refer you to an excellent summary of these issues here by IBCLC Meg Nagle who has covered the bases on this one. So is there reason to worry about solitary sleep? For some families, yes. And this highlights one of the most frustrating parts of this research: the lack of nuance. On top of simply ignoring mother-infant biology, the researchers blithely ignore that families have their own considerations that can make any sleeping arrangement problematic. One of the things the recent AAP guidelines tried to do (though still fell far short, in my opinion) was to create a bit of nuance to allow caregivers to work with people instead of rules. Frankly we would all be better off if that approach was taken in any discussion of infant sleep. ______________________ The first thing we need to look at is what kind of data collection are we looking at here. The data comes from the INSIGHT study which is an ongoing, prospective, randomized, controlled trial evaluating an intervention to prevent childhood obesity. Families in the Pennsylvania area are recruited and randomly assigned to either a control group or intervention group. As described on the study’s site, “The parenting intervention messages are related to responsive feeding, division of feeding responsibility, and healthy dietary choices designed for the prevention of obesity that extend from infancy through age 3 years. These materials also contain messages relating to sleep, active social play, and child fussiness/soothing. The control group receives messages focused on the safety of the child’s environment and interaction with parents.”
The first thing we need to look at is what kind of data collection are we looking at here. The data comes from the INSIGHT study which is an ongoing, prospective, randomized, controlled trial evaluating an intervention to prevent childhood obesity. Families in the Pennsylvania area are recruited and randomly assigned to either a control group or intervention group. As described on the study’s site, “The parenting intervention messages are related to responsive feeding, division of feeding responsibility, and healthy dietary choices designed for the prevention of obesity that extend from infancy through age 3 years. These materials also contain messages relating to sleep, active social play, and child fussiness/soothing. The control group receives messages focused on the safety of the child’s environment and interaction with parents.”
Looking at the study methodology in depth, I want to highlight a few things that cause concern:

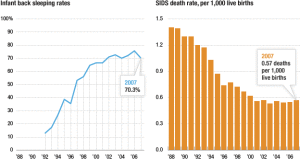
While I actually appreciate their thoroughness in this regard, I want to point out some of the flaws in their own reasoning here:
Should babies sleep alone? An Analysis of the INSIGHT Study’s Findings on Infant Sleep by Location
[1] has been making the rounds as the authors make the suggestion that the American Academy of Pediatrics’ recommendation that all babies room-share for the first year of life to reduce SIDS is unfounded and has possible negative consequences for sleep. As the authors themselves put it in the abstract of their article






CAn you please submit this as a letter to the editor?!?!? This needs to be said in the same forum as the original article because it is brilliantly written and logical.
OMG you are my hero. Thank you for breaking this down. Always appreciated.
‘Parent reported’. Whenever I hear any study or individual account when parents report their child ‘slept through the night’ at some absurdly young, physiologically speaking, age, all I hear is “I sleep through my baby waking up”. Of course ‘I sleep through my baby waking ‘ pretty much means anything past that is useless.
The other thing, however, is one that rarely gets brought up: we assume that baby sleeping for longer stretches is better because parents in an industrialized culture prefers them to sleep longer. But that’s a huge assumption, and one that really doesn’t seem to be supported by either history or physiology. Even IF (and obviously that’s a huge if) babies did sleep for longer stretches in a solitary environment, that says zero about whether that is better for their development and normal physiology. It seems to be quite the opposite, as long stretches sleeping without waking to feed is a known risk factor of unnaturally early weaning from the breast and even failure to thrive. So at best all these books, studies, and plans to make babies sleep through the night propose putting babies into an unnatural situation (solitude) to cause another unnatural situation (excessive infant sleep).
Thank you, this was an excellent article! I think we totally focusing on the wrong things in the Western world, when we somehow see ourselves as successful parents when our kids DON’T need us. Babies should sleep through and alone, wean early, self-soothe and play nicely on the floor on their own – when exactly the opposite are signs of strong bonds and (I think) a more natural development path for the child.
Amen, I have been saying this for years now. Any sleep situation can be problematic. However, when you breastfeed it is best to have the baby at least in your room for the first few months of their life. My oldest slept in the bed with us until he was 6 months old and the only reason why he stopped is one he was sleeping through the night and two because he is a bed hog lol. My youngest did not sleep in the bed with us much but he slept right next to me in his crib. I could easily roll over and get him at anytime. It should be what the baby needs are. I feel as though some of these people do these studies and are not parent’s themselves. Because if they were parent’s they would know that sometimes to get sleep yourself you have to put the in bed with you or be up all night. Good article.
I am so glad to have found your site! I had major sleep issues with my first, where I tried desperately to get him to sleep all night in his crib. Now 10 years later I had my second and I am co-sleeping and following many of the evolutionary parenting principles. By no means am I not woken in the night, but I feel much more rested (at nearly age 42 no less). I am woken by a restless baby and put him to the breast right away and he is right back to sleep. Happens about 3 times per night but I am much less stressed about it then being FULLY woken by a FULLY awake baby in a crib. Thank you Dr. Cassels for your work, especially with your criticism of Baby Wise. I hope your work reaches millions.
Thank you!!! I’m so happy to hear you enjoying baby time and sleep time more the second time around 🙂