In a new study that should come as a surprise to no one, researchers at Centenary Hospital in Australia examined the influence of a policy that enabled earlier release of tongue-ties on breastfeeding and found that the early release of the tongue-tie had a significant impact on breastfeeding success
To examine this, let’s take a closer look at the actual study. The study compared cohorts of births at this particular hospital from 2008 and 2011. Since 2007, the hospital has had a policy to divide tongue ties as soon as it is clear that it is posing a difficulty for feeding; however, in 2011, this policy was modified in that it now included the caveat that the tie should not be divided until it was clear the cause was not something else and could not be cut until after 7 days. The basis was the fear of unnecessary pain associated with the cutting or lasering of the tie and making sure the proper diagnosis was given.
However, previous research on the effect of moderate-severe tongue-ties on breastfeeding has found that the effect is quite immediate with a significant proportion of women giving up breastfeeding in the first week when their infant has a tongue-tie[2]. Thus, the question becomes, what kind of effect would a policy that delays when the tie is divided have on breastfeeding?
The comparison of births between 2008 and 2011 found that there were no differences in the rates of tongue-tie identified and released (both were around 5%), birth weight of the babies with tongue-tie, gestational age, or sex. However, the significant differences began with the age at which the tongue-tie was divided, or released. In 2008, before the implementation of the new policy that required a wait, ties were released on average 6.5 days after birth (with a range of 2 to 11 days); however, in 2011, after implementation, the average age of release was 9.7 days (with a range of 3.5 to 16 days).
Some might be thinking this difference of 3 days really shouldn’t be that much of a big deal. After all, if it’s caught, then things will be fine, right? Especially in the first two weeks of life. Not so. First, there was the issue of pain for the mothers in which 85% of moms in 2008 reported significant nipple pain compared to 97% in 2011. This suggests that delaying the release results in greater pain for mom and if mom is in a lot of pain, what is likely to happen?
If you guessed “Give up on breastfeeding”, give yourself a gold star. This is exactly what was found. In 2008, by the time the tie was cut, only 3.5% of moms had given up breastfeeding in favour of exclusive pumping and/or formula use, but this increased to 17.4% in 2011. Importantly, once the tie was released, the nipple pain reported ceased nearly immediately for the majority of women, meaning the earlier this is caught, the more likely they are able to salvage or maintain a breastfeeding relationship.
Although some of the women were able to regain a breastfeeding relationship after the tie was divided, there are greater difficulties associated with releasing the tie at a later date, including reduced breastmilk supply, engorgement, mastitis, and difficulty re-establishing breastfeeding due to latch problems after the use of a bottle so early[2]. There is also, as the authors rightfully point out, “the emotional trauma for the mother of having to feed in a different way to her chosen method” ([1], p.14). The authors conclude that tongue-ties should ideally be identified and released by 72 hours post-birth in order to have minimal effect on the breastfeeding relationship and I, for one, hope that hospitals and professionals around the world take note.
How do I know if my child has a tongue-tie?
There are certain signs and symptoms you can look for and notice pretty quickly, but the end diagnosis must be made by a professional who can cut or laser the tie. In the USA, Dr. Larry Kotlow is considered one of the foremost experts on identifying (and releasing) tongue-ties and he has created some great visuals and videos to help families, which I share here.
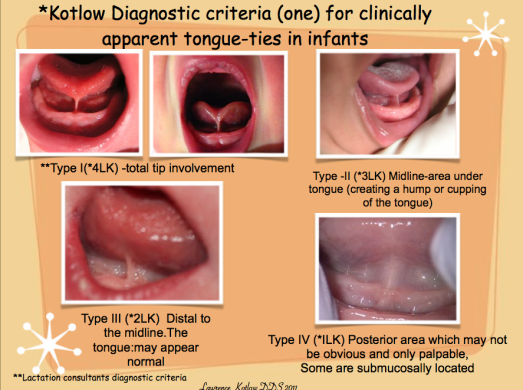
The first is an image of what to look for in the four main types of tongue-tie:
Note that a fifth type of tie has been identified in the research literature, but very few clinicians currently use it during diagnosis. Type 5, or “submucosal” tongue-tie[1], is another posterior tie (like type 4), but is located greater than 15mm from the tip of the tongue (as opposed to the 11-15mm for a type 4). It is thin and shiny when the tongue is elevated. Like all posterior ties, it is difficult for parents to truly feel confident in knowing if their child has one or not and thus having it checked out is a must. However, here is a video from Dr. Kotlow on how to check your child for a posterior tongue tie in case you are wanting to check it out:
In addition to the visual checks, there are signs and symptoms that moms and babies show that are often (though not always) indicative of a tongue-tie. Again, others have created great images so I will share one from MommyPotamus here so you can see what kind of symptoms are associated with tongue-ties for both mom and baby.
As the research shared above highlights, if you can, get this dealt with as soon as possible. There is no need to suffer through pain and bad latch and no need to risk your breastfeeding relationship. Yes, there will likely be a small amount of pain when it is released, but the paediatric dentist will tell you exactly how to minimize that if a release is necessary.
Are there long-term effects of tongue-ties if they aren’t released?
The most common long-term problem with tongue-ties is speech-related. The tongue-tie causes a restriction of movement which makes speech difficult for children as they age. Children with tongue-ties may have a delay in speech onset as well as difficulty pronouncing certain sounds and words. If you are going to see a speech therapist, make sure that either you or the therapist checks for a tongue-tie first as this should be released before embarking on therapy.
A second long-term issue is to do with how teeth come in, resulting in higher likelihood of dental work later on. As reported by Breastfeeding USA, tongue-ties can result in front, bottom teeth being pulled into the mouth, narrow palates, and overcrowding of teeth. Expensive (and possibly painful) dental work is a very good reason to get a tie released early.
What about lip-ties?
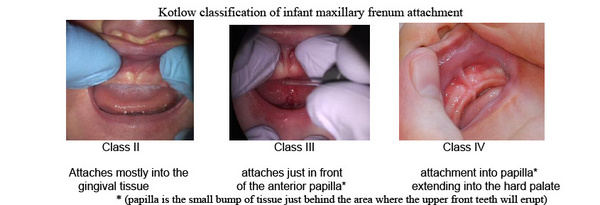
In addition to tongue-ties, there are lip-ties that can also influence breastfeeding. Again, from Dr. Kotlow, you can see what a lip-tie looks like and how to diagnose it:
Now, it’s worth noting that if you see a lip tie, there will almost always be a tongue-tie as well, though not vice versa. Although lip-ties will affect breastfeeding as the baby can struggle with latch as the lips don’t properly open up, it is not associated with later speech problems so if you made it through the breastfeeding period, you will likely not worry about releasing it later.
There is a caveat to this, though, in that the lip ties can be associated with spacing between the front teeth if the tie is severe enough which can cause the need for orthodontic work later. If you see this happening, your dentist may recommend a release at a later age. Also, there is a higher likelihood of cavities on either side of the tie as food is pushed into the pockets of the side of the tie.
Who do I see about a tongue-tie or lip-tie?
Often families go to their paediatrician in hopes of getting a tongue-tie diagnosed, but this is not the person you want to see. Not saying there aren’t paediatricians out there who could accurately diagnose a tongue-tie, but they are few and far between, yet many families report these doctors – who are well-versed in so many areas – giving false information about ties.
No, for a tongue-tie, the people you want to see are either a lactation consultant (preferably an IBCLC as they have specific training) or a paediatric dentist. The foremost “experts” in most countries are paediatric dentists as their specialty is the mouth and they can readily identify most ties (of course, as always, some are better than others). You want to make sure that you find someone who clearly advertises their tie expertise and their commitment to breastfeeding when you’re looking for a paediatric dentist to examine a tie. You also want to ask your LC if they have experience in this regard as not all are equally adept at identifying some of the harder (i.e., posterior) ties.
Many paediatric dentists who specialize in ties will do a consult for a low fee ($50) and then can release the tie that very day if they identify one that requires releasing. An LC can identify the tie and refer you to someone to conduct the release, but will not do the release her/himself. However, an LC is a great source for a good referral as they are likely to know the top specialists in the area.
____________________________________
[1] Todd DA, Hogan MJ. Tongue-tie in the newborn: early diagnosis and division prevents poor breastfeeding outcomes. Breastfeeding Review 2015; 23: 11-16. [2] Hogan MJ, Westcott C, Griffiths M. Randomized, controlled trial of division of tongue-tie in infants with feeding problems. Journal of Paediatric Child Health 2005; 41: 246-50.







Great article! Do you have any good references re: ties and speech issues? I’ve heard that these are frustratingly sparse.
Very sparse! I actually learned most from the paediatric dentist whom I spoke to. If I come across something good I’ll share here 🙂
Thanks 🙂
Excellent article!
Please note that:
– The link to Larry Kotlow goes to a different pediatric dentist in PA.
– The link to Breastfeeding USA should go to
https://breastfeedingusa.org/content/article/tell-me-about-tongue-ties
1) The Kotlow one is the right link for me – the Dr. Kotlow in Albany, NY. You don’t get that???
2) I meant for it to go to the main page as the site is a wealth of information 🙂
This article provides some excellent information about tongue-ties and lip-ties in infants and the research findings validate my own beliefs about the importance of early diagnosis AND treatment of restrictive tongue-ties to preserve the breastfeeding relationship. Having said that, I emphasise the importance of skilled breastfeeding support to address and guide all aspects of the mother and baby’s breastfeeding struggles. Enabling baby to respond to his instinctive feeding behaviours, and development of mother/baby skills to achieve an optimal deep latch is essential in every breastfeeding relationship. Releasing a restrictive tongue-tie if it exists – earlier rather than later – will always help the process. Unfortunately it is often the case that the focus is on the tongue-tie release and there is a lack of prior and ongoing breastfeeding support. I also believe as awareness about “posterior tongue ties” has grown many babies are being diagnosed has having PTTs and LTs by parents and others who are not qualified to do so. Consequently many invasive and expensive laser treatments are being performed by dentists which are NOT necessary or helpful to baby or the breastfeeding mother. The large numbers of PTT and LT laser procedures which are proudly displayed on some dentists’ websites are proof that over-treatment IS occurring – their numbers just don’t match the epidemiological incidence of true PTTs. Think carefully and get expert breastfeeding support before you go ahead with invasive painful laser treatments in your infant’s mouth as it might not be necessary. Lois Wattis IBCLC and Clinical Midwife.
Thank you Lois. I have had two well-fed, uncut tongue-tied babies. This is after having one horrible breastfeeding experience, and then lots of support to have great experiences there after. With the first TT baby I only knew because a doctor told me long after he was a newborn. With the second TT, I also found out after googling why she made clicking sounds when she nursed. It’s unfortunate to see these variations seen as deformities which *may* cause problems instead of natural variations. But absolutely, the key is overall more breastfeeding support.
The latest AAP article advocates waiting, and trying other methods like CST. I had a difficult time finding the citations they used, which also were quite old. Hmmmmm
The specialist in my area was actually an ENT, ear nose and throat Doctor.
I cannot speak highly enough of getting it clipped. My son’s was diagnosed at 8 weeks after a case of “thrush” that just wouldn’t go away actually was nerve damage to my nipples. Immediate improvement after lasering, but he never learned to have a deep latch.
When I mentioned it to the pediatrician at his next visit: “oh, I noticed the tie earlier but since he was gaining weight I didn’t mention it.”
Really disappointed to see EP join the Group Think.
We had severe breastfeeding problems since birth – I had a lot of pain, cracked nipples, decreasing milk supply and the baby was irritable, always hungry, fussy at breast and had poor weight gain. At 7 weeks we were seen by a lactation consultant, who suggested there may be a posterior tongue-tie (neither our GP nor anyone in the hospital recognised it, though) and were referred to a specialist. The tongue-tie was released at 9 weeks, a tiny cut of about 2 mm (not lasered, just a small pair of scissors and experienced hand of the specialist). For about a week, the problem was even worse. But then, all of a sudden, it miraculously fixed. One morning my baby just latched on her own, I felt no pain and she was drinking beautifully and for the first time in her life she seemed content after the feed. If only there had been someone at the hospital able to identify a posterior tongue tie and released it stright away!